RSM Blog: Manual Therapy Techniques
Shiatsu Massage for Postpartum Recovery: Integrating Eastern Modalities with Sports Medicine
The Physiological Reality of the Fourth Trimester
The human body undergoes no greater singular physical transformation than the process of gestation and parturition. In the span of roughly forty weeks, the musculoskeletal architecture shifts entirely; the center of gravity migrates, the pelvic girdle expands, and the hormonal landscape floods with relaxin to facilitate tissue laxity. Once the birth event concludes, these adaptations do not simply vanish. Instead, the body enters a distinct rehabilitative phase often termed the "fourth trimester," a period characterized by acute structural recalibration and significant demands on the autonomic nervous system.
At RSM International Academy, we approach this phase not merely as a time for relaxation, but as a critical window for soft tissue rehabilitation. While standard Western physiotherapy focuses heavily on restoring pelvic floor integrity, the manual therapy component – specifically the application of static pressure techniques found in shiatsu massage – offers a unique mechanism for addressing the hypertonicity and fascial restrictions that accompany new motherhood.
Managing Pain and Structural Realignment
The primary complaint we encounter in postnatal recovery is rarely limited to a single site; it is a systemic pattern of compensation. During pregnancy, the increasing weight of the uterus pulls the lumbar spine into lordosis. Following childbirth, the sudden absence of this anterior weight creates a vacuum of stability. The abdominal wall struggles to support the lumbar curve, leading to persistent pain and lower back discomfort.
Simultaneously, the mechanics of caring for a baby introduce new repetitive strain patterns. The act of breastfeeding or bottle-feeding typically induces a thoracic kyphosis and protracted shoulders. This posture shortens the pectoralis minor and places eccentric strain on the rhomboids.
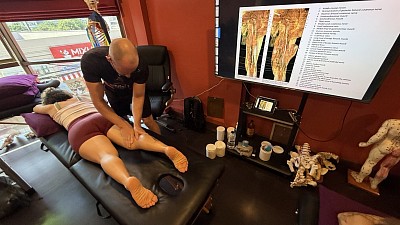
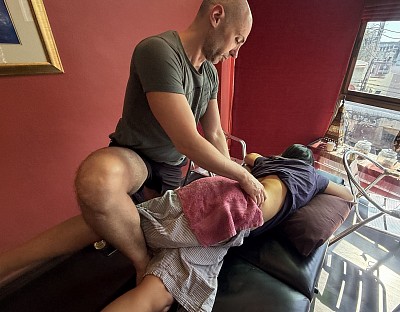
In a clinical setting, addressing this requires a restoration of proprioceptive balance. We utilize Shiatsu to access the paravertebral muscles along the Bladder meridian. By using sustained, rhythmic pressure here, we encourage the erector spinae to release hypertonicity without forcing the vertebral joints into unsafe positions. This approach respects the structural vulnerability of the mother while effectively mitigating the muscular tension that exacerbates chronic discomfort.
The Mechanics of Shiatsu Massage
The technical distinction of Shiatsu lies in its application of force. Unlike Swedish massage, which relies on friction and oil to manipulate the dermal layers, a shiatsu technique functions through compression. For a postpartum client, this distinction is clinically significant. The use of oil can be impractical for women dealing with hormonal night sweats or body image sensitivities. Shiatsu is traditionally performed with the client fully clothed, often on a floor mat, providing a sense of grounding that is essential for psychological safety.
From a sports medicine perspective, the static pressure acts on the mechanoreceptors within the fascia. When we apply pressure, we create a temporary ischemia followed by a reactive hyperemia upon release. This flushing effect improves local circulation, aiding in the removal of metabolic waste from fatigued tissues. Furthermore, steady pressure stimulates the vagus nerve to promote relaxation, shifting the system toward parasympathetic dominance – the state in which tissue repair occurs most efficiently.
We often observe that the tactile input provided by Shiatsu helps reintegrate the client’s sensory map. After the physical trauma of labor, particularly if medical interventions were necessary, a woman may feel dissociated from her pelvic region. Careful palpation helps the brain re-establish connection with these areas, a vital step in motor control recovery.
Targeted Pressure Points and Safety Protocols
Safety is paramount when treating this population. The presence of relaxin can persist in the body for months after weaning, meaning joint capsules remain susceptible to overstretching. A shiatsu practitioner must be acutely aware of these limitations, avoiding aggressive joint mobilizations that might destabilize the sacroiliac joint.
Instead, we focus on specific pressure points located in the muscle bellies to provide pain relief:
- Gallbladder 21 (Jian Jing): Located at the apex of the trapezius. This point is critical for releasing neck tension derived from nursing posture. While contraindicated during pregnancy, it becomes a primary target for relief postpartum.
- Large Intestine 4 (He Gu): Found in the webbing between the thumb and index finger. New mothers frequently suffer from De Quervain’s tenosynovitis due to the lifting mechanics of holding an infant; treating this point can alleviate strain in the wrist complex.
- Stomach 36 (Zu San Li): Located on the lower leg. This point is renowned for boosting immune function and digestive energy, combating the systemic fatigue that defines the postpartum period.
While acupuncture accesses these points via needles, Shiatsu uses the thumbs and palms. This broader contact surface is often more reassuring to a sensitised nervous system, allowing us to modulate intensity in real-time.
Optimizing Emotional Well-being and Nervous System Regulation
The exhaustion inherent in the early months of parenting is a state of deep depletion. In Western physiological terms, we might correlate this with adrenal fatigue or the metabolic cost of lactation. The nervous system remains in a heightened state of alertness, constantly scanning for the needs of the infant, often leading to anxiety.
Therapeutic intervention must prioritize the sedation of the nervous system. If we attempt aggressive deep tissue work on a system that is alarmed, the body will guard against it. Shiatsu’s rhythmic pacing mimics the physiological rhythms of the breath and heartbeat, entraining the client’s system into a restorative cadence.
We consider the treatment room an extension of the recovery ward. By targeting points along the Kidney and Bladder meridians, channels traditionally associated with constitutional vitality, we aim to support the mother’s baseline energy reserves. This leads to a measurable reduction in cortisol levels and an improvement in sleep quality, both of which are prerequisites for health and physical healing.
Clinical Considerations and Conclusion
We must rigorously screen for red flags before commencing treatment. The risk of Deep Vein Thrombosis (DVT) remains elevated in the weeks following birth. Any signs of heat or swelling in the calves require immediate medical referral. Furthermore, we frequently utilize the side-lying position, which is neutral for the spine and permits access to the back without compressing the chest or abdomen.
The benefits of integrating Shiatsu into the recovery plan extend beyond immediate symptom relief. By addressing postural deviations early, we prevent them from becoming chronic structural patterns. The "nursing hunch" of today can become the hyperkyphosis of next year if the pectorals are not released. Moreover, this work supports the efforts of pelvic floor physiotherapists by ensuring the external musculature does not compromise pelvic alignment.
In many cultures, the period following birth is protected by a community. In our modern context, this is often lacking. Manual therapy bridges this gap. For the sports medicine professional, mastering this application expands the scope of practice to include a demographic critically in need of skilled touch.
(For those interested in mastering the clinical application of these techniques, our Shiatsu Massage Course provides comprehensive training in biomechanics and meridian therapy.)
Key Takeaways for Practitioners
- Screen for Clotting: Always assess for DVT symptoms.
- Respect Relaxin: Avoid end-range stretches; focus on stability.
- Positioning: Utilize side-lying positions to accommodate breast tenderness.
- Autonomic Regulation: Prioritize slow, rhythmic pressure to sedate the sympathetic nervous system.
At RSM, we believe the most effective therapy honors the complexity of human physiology. By combining the precision of sports medicine with the holistic scope of Shiatsu, practitioners can offer improved outcomes for recovery and long-term well-being.
The Role of Remedial Massage for Stress Management in Modern Therapy
The human body possesses an antiquated alarm system for a modern environment. The hypothalamus-pituitary-adrenal (HPA) axis does not distinguish between the immediate threat of a predator and the sustained pressure of a corporate merger. In both instances, the physiological response is identical: a flood of cortisol, increased muscle tone, and a rapid heart rate. When this "fight or flight" response becomes chronic, the cost is systemic inflammation and musculoskeletal dysfunction.
In my work training medical professionals and manual therapists at RSM International Academy, I often encounter a division between physical treatment and psychological support. We treat the shoulder, or we treat the mind. Yet, this dichotomy is false. The nervous system governs the musculoskeletal system; therefore, effective manual therapy must address the neurological state. We are not merely treating muscles; we are modulating the autonomic nervous system.
The Neurobiology of Massage Therapy
To appreciate the utility of massage in a medical context, one must look beyond the relaxation paradigm often sold by the spa industry. While relaxation is a byproduct, the primary mechanism of remedial work is the downregulation of the sympathetic nervous system.
The skin is the body’s largest sensory organ, densely populated with C-tactile afferents. These nerve fibers are tuned specifically to slow, low-force mechanical stimulation and project directly to the insular cortex – the brain region responsible for interoception and emotional regulation. When a massage therapist stimulates these receptors, they are effectively hacking the stress response loop. Research confirms that this stimulation reduces cortisol circulation while increasing serotonin and dopamine.
This is why massage therapy is a viable intervention for mental health challenges like anxiety and depression. It is a neurochemical intervention delivered through the hands. When we reduce nociceptive signals (pain signals) from hypertonic tissue, the brain deprioritizes the threat response. This lowers global stress levels, allowing the patient to shift into a parasympathetic state – the "rest and digest" mode where true tissue repair occurs.
Clinical Application of Massage Techniques for Stress Relief
The application of massage techniques for stress relief requires a sophisticated understanding of pacing and pressure. In sports medicine, we often utilize vigorous friction to remodel scar tissue. However, when the clinical objective is autonomic regulation, the approach must shift.
Deep tissue work is highly effective for reducing chronic stress, but only if the nervous system perceives it as safe. Rapid, aggressive strokes trigger defensive guarding, a sympathetic spike that is counterproductive. Conversely, slow, sustained pressure into the fascia allows mechanoreceptors to signal safety to the brain. An expert therapist waits for the tissue to yield rather than forcing it.
We often use elements of Swedish massage, such as rhythmic effleurage, as a neurological bridge. These strokes habituate the patient to touch, lowering their defensive threshold. Once this safety is established, we can apply ischemic compression to release stored tension. The release of a trigger point often brings a profound sense of relief that is both physical and emotional, suggesting that muscle tension acts as a somatic container for psychological strain.
Remedial Massage for Postural Correction
The body keeps a meticulous record of psychological load. We see this in the "startle pattern" locked into the posture of high-stress professionals: internal rotation of the shoulders, forward head carriage, and a collapsed chest. This posture mechanically restricts the diaphragm, forcing the patient into shallow, apical breathing.
Apical breathing recruits accessory muscles like the scalenes and sternocleidomastoid, which are ill-equipped for the constant load of respiration. This leads to chronic neck pain and tension headaches, feeding back into the anxiety loop. A patient who cannot breathe deeply cannot relax physiologically.
Here, remedial massage becomes a critical tool for wellness. We must manually lengthen the pectorals and mobilize the thoracic spine to allow the ribcage to expand. Simultaneously, we treat the diaphragm and intercostals. By mechanically creating space for the breath, we facilitate a shift in the patient's physiological state.
This mechanical restriction is often overlooked in standard psychological treatments. While talk therapy addresses the mind, manual therapy addresses the vessel. For practitioners looking to master these structural integrations, the Remedial Massage Course at RSM offers a curriculum designed to bridge the gap between structural bodywork and systemic health. We teach that you cannot talk a patient out of a panic attack as effectively as you can manually facilitate a deep breath.
The Therapist’s Role in Regulating Stress
For the medical professional or massage therapist, integrating these concepts requires a shift in assessment. We are not just treating localized conditions; we are treating a system under load.
During a session, the practitioner must evaluate autonomic tone. Are the patient’s hands cold? Is muscle tone universally high? These are signs of sympathetic dominance. In such cases, the benefits of treatment are maximized by focusing on the spine and craniosacral system. The paraspinal muscles house a high concentration of muscle spindles; reducing tone here has a global calming effect on the nervous system.
Furthermore, the state of the therapist is a tangible variable. To regulate another human's nervous system, the therapist must be regulated themselves. "Therapeutic presence" is the quality of attention that allows a patient's body to detect safety. If the therapist is rushed, the patient’s system will refuse to yield.
The Long-Term Impact of Remedial Therapy
We must recognize that stress is a precursor to pathology. By the time a patient presents with hypertension or autoimmune issues, the dysregulation has likely been present for years. Massage offers a unique window of intervention. It is one of the few modalities that can manually override the sympathetic driver and force the system to pause.
This is not a passive luxury; it is an active, remedial intervention that restores the capacity for self-regulation. When we reduce pain and tension in the physical structure, we lower the noise in the nervous system. The body and mind are not separate entities to be treated in isolation. As we advance our understanding of the human organism, the role of intelligent, clinically reasoning manual therapists becomes central to comprehensive healthcare. We do not just manipulate tissue; we reshape the environment in which the mind resides.
How to Improve Palpation Skills: Beyond Basic Anatomy
The human hand is a biological marvel, capable of detecting surface irregularities as small as 13 nanometers. Yet, in sports medicine and manual therapy, this incredible sensitivity is often rendered useless by a lack of interpretive framework. When I observe students at RSM International Academy, the difference between a novice and a master is rarely the sensitivity of their fingertips. It is the clarity of their mental map. To refine the art of touch is to refine the mind; one must learn to "see" with the hands by anchoring sensation in rigorous anatomical logic.
Touching a patient is easy; understanding what you are touching is a career-long pursuit. Many practitioners plateau because they rely on pattern recognition rather than active interrogation of the tissue. They feel "tightness" and apply pressure, assuming the hypertonicity is the issue rather than a symptom. True improvement requires shifting from passive reception to active inquiry.
The Role of Clinical Reasoning in Touch
We often treat palpation as a physical act, but it is primarily cognitive. The fingertips are data collectors; the brain is the analyst. If the analyst has incomplete data, the conclusion will be incorrect regardless of the input quality. This is where clinical reasoning becomes the scaffold for assessment.
When I place my hand on a patient, I am asking binary questions. Is this tissue warm or cool? Is the texture consistent with fluid stasis or fibrous adhesion? Does the tension change when the joint is moved? This internal dialogue transforms a massage session into a clinical investigation.
New students often rush into deep work before the nervous system has granted access. To elevate your practice, you must slow down. You must train your brain to filter the noise of general sensation and isolate specific variables. When you visualize the striation of the muscle fibers or the depth of the lamina while you touch it, your brain tunes the gain on the signal coming from your receptors. You begin to feel what you know.
Implementing a Seven-Step Palpation Strategy
In high-pressure sports medicine, where a misdiagnosis can cost an athlete their season, we cannot rely on intuition alone. We need a systematic protocol. At RSM, we advocate for a seven-step palpation routine to ensure no variable is overlooked.
- Visual Observation: Assessment begins before contact. We look for asymmetry, discoloration, or swelling. Visual data primes the brain for what the hands should expect.
- Temperature Assessment: The dorsum of the hand scans for heat (acute inflammation) or cold (ischemia). Temperature dictates the intensity of subsequent work.
- Superficial Fascia and Skin Mobility: We assess the glide of the skin over the underlying fascia. If the skin does not glide, deep pressure will only cause shearing pain.
- Muscle Tone and Texture: We differentiate between protective muscle guarding (active engagement) and intrinsic hypertonicity (structural hardness).
- Bony Landmarks and Alignment: Palpation must anchor to the skeleton. Misidentifying a landmark is the most common cause of error.
- Trigger Point Identification: We hunt for specific hypersensitive loci and referred pain patterns, distinct from general tone.
- Provocation and Motion: We palpate while the tissue is in motion (active or passive).
By adhering to this step palpation hierarchy, we build a composite picture of dysfunction, layer by layer, rather than chasing pain.
Refining the Palpation Method through Mechanics
The mechanics of force application dramatically alter the data received. Many therapists rely solely on heavy compression, which often obscures subtle textural changes. To improve, one must vary the palpation method based on the target structure.
Consider the angle of incidence. Direct perpendicular pressure is excellent for assessing muscle belly density but poor for fascial restrictions. To detect adhesion, we must use shear force by applying pressure at a 45-degree angle. This activates different mechanoreceptors, allowing us to feel the drag of the connective tissue.
The surface area also matters. A broad palm offers global assessment but lacks resolution. The fingertips offer the highest density of sensory nerve endings. However, sharper pressure can trigger guarding. The solution is "sinking." Instead of forcing through layers, we match the tissue's tension and wait for the nervous system to accommodate. As the tissue relaxes, we sink deeper. This is an active negotiation with the patient’s defensive reflexes.
Differentiating Tissues: The Art of Texture
Anatomy books are color-coded; bodies are not. In a living patient, structures blend. The ability to distinguish a tendon from a nerve is the hallmark of advanced palpation skills.
Muscle is viscoelastic; it deforms under pressure and slowly returns to shape. When a therapist detects a taut band, it represents fibers stuck in a contracted state. Tendons, conversely, are denser and less compliant. Differentiating them requires tracing the structure to its attachment. If it transitions into bone, it is tendon; if it broadens, it is muscle.
Ligaments are difficult to isolate as they are often buried deep within the capsule. They feel like leather straps; tough and unyielding. To confirm you are on a ligament, you must stress the joint. If the structure tightens at the end-range of passive motion, you have likely isolated it.
Nerves present a unique signature, often feeling like firm, cooked spaghetti. Unlike other tissues, nerves are extremely sensitive to compression. If a patient reports a sharp, electric sensation, immediate adjustment is required. Knowing exactly where nerves traverse the anatomy is non-negotiable for safety.
Active vs. Passive: The Diagnostic Nuance
Static palpation only tells half the story. The body is designed for action, and dysfunction often reveals itself under load. We utilize diagnostic palpation to differentiate between structural shortening and functional guarding.
For example, if a hamstring feels tight while the patient is prone, we ask them to slightly lift their lower leg. If the texture changes dramatically during this active movement, the issue is likely neurological. If it remains rock hard, we are dealing with structural fibrosis. This dynamic approach uses the patient's own physiology to enhance the resolution of your touch.
Overcoming Perceptual Bias
The brain is a pattern-matching machine that wants to find what it expects. This leads to perceptual errors – feeling things that aren't there because the diagnosis is already decided in the mind.
To combat this, we must remain agnostic. If I find a tender spot, I do not immediately label it the source of the pain. I look for disconfirming evidence. True clinical excellence requires intellectual humility. The sensation of a "knot" can be caused by edema, fascial thickening, or referred sensation. By cross-referencing tactile findings with orthopedic testing, we reduce the margin for error.
The Feedback Loop: Practice and Validation
Reading about palpation does not replace the hours of practice required to build tactile memory. However, blind repetition is insufficient. You need a feedback loop.
In the clinic, validation comes from the outcome. If you believe you have released a restriction, re-assess. Has the range of motion improved? If the objective markers haven't changed, the palpation was likely off-target. It is also vital to palpate "normal" tissue first to establish a baseline. "Tight" is a relative term; comparison is the basis of assessment.
Integrating Knowledge for Advanced Therapy
Palpation is the bridge between theoretical anatomy and the living human on your table. It is where science meets sensation. At RSM, we view medical massage not as a set of techniques, but as a philosophy of care grounded in accuracy. We drill anatomy until it is second nature, so that when your hand lands on a patient, you are verifying rather than guessing.
For those looking to deepen their understanding, our curriculum focuses on integrating diagnosis and treatment. The nuances of identifying deep anatomical structures are explored extensively in our Deep Tissue Massage Course. This training moves you past the basics of "rubbing where it hurts" and into true structural correction.
Learning to palpate is a continuous evolution. The body is infinitely complex, and no two patients are identical. Improvement requires a commitment to never being satisfied with a superficial understanding. By systematizing your approach, refining your mechanics, and engaging in constant research of your own results, you elevate your work from simple interaction to profound intervention. The hands are capable of miraculous things, but only when guided by an educated mind.
Integrating Trigger Point Therapy in Practice for Modern Clinicians
Pain is rarely where it claims to be. A patient presents with a searing headache behind the eye, yet neurological testing is clean. Another arrives with deep joint pathology in the shoulder, mimicking bursitis, yet imaging reveals structurally sound tissues. For the clinician standing at the intersection of modern sports medicine and manual therapy, these moments are not dead ends; they are invitations to look elsewhere. They are often the silent signals of myofascial dysfunction.
In my years founding RSM International Academy and navigating the complexities of sports medicine, I have found that the most profound shifts in patient outcomes often come from addressing the invisible architecture of the musculature. The hyperirritable spot, the taut band, the localized twitch: these are not merely nuisances to be rubbed away. They are physiological blockages that disrupt the kinetic chain.
For the serious practitioner, whether a physiotherapist, doctor, or advanced bodyworker, the challenge lies in moving beyond the basic "search and destroy" mentality. The true art lies in high-level clinical reasoning. It requires understanding the physiological cascade of the energy crisis within the sarcomere and recognizing how pain referral patterns masquerade as other pathologies. This is the foundation of trigger point therapy in practice.
The Physiology of the Myofascial Trigger
To treat effectively, we must first respect the mechanism. A trigger point is not simply a hard patch of muscle. It is a microscopic failure of localized physiology. Current research supports the "Integrated Trigger Point Hypothesis," often describing a metabolic crisis at the neuromuscular junction. When a muscle fiber is subjected to repetitive overload or acute trauma, acetylcholine release can become excessive, flooding the synaptic cleft and causing a continuous release of calcium ions.
The result is a sustained contraction of the sarcomeres. This contraction compresses local capillaries, restricting blood flow and effectively starving the tissue of oxygen. Without oxygen, the muscle cannot produce enough ATP to release the contraction. The muscle is locked in a metabolic deadlock.
This creates a toxic chemical environment. Sensitizing substances accumulate, lowering the firing threshold of nociceptors. This is what we feel under our fingers: a distinct, ropy texture within the muscle belly. By visualizing this microscopic crisis, we change how we touch. We are intervening in a chemical feedback loop to mechanically separate the actin and myosin, restore local perfusion, and flush the sensitizing substrates. This understanding elevates the work from simple massage to clinical medicine.
Differentiating Trigger Points from General Tension
Not every tight muscle houses a trigger point. Distinguishing between general hypertonicity and a discrete myofascial trigger point is a requisite skill for the advanced therapist. Hypertonicity usually involves the entire muscle and releases with general stretching. A trigger point is focal.
We look for three defining characteristics during palpation: the existence of a taut band within the muscle fibers, a tender nodule along that band, and the patient’s recognition of the pain as their "familiar" pain.
Crucially, we must distinguish between active and latent points. An active trigger point causes spontaneous pain even at rest. A latent trigger point is silent until provoked by pressure. Latent points are treacherous in a clinical setting; they do not produce spontaneous pain, so the patient does not complain of them, yet they still restrict range of motion and cause muscle weakness. In a high-performance athlete, a latent point in the gluteus medius might inhibit firing enough to alter gait mechanics, eventually causing a knee injury downstream.
Dry Needling vs. Manual Therapy
In the landscape of modern intervention, the debate between manual compression and invasive techniques is ongoing. Dry needling has gained significant traction in physiotherapy circles. The insertion of a filiform needle directly into the trigger point can elicit a vigorous local twitch response, effectively resetting the neuromuscular junction.
However, dry needling is not always the superior option. Manual trigger point therapy offers benefits that needles cannot replicate. The tactile feedback loop between the therapist’s hands and the patient’s tissue provides real-time data on tissue compliance and fascial glide.
When I treat, I use my hands to listen. Manual ischemic compression – applying sustained pressure to the point – creates a reactive hyperemia. When the pressure is released, fresh, oxygenated blood rushes into the hypoxic zone. While injection therapy and dry needling have their place in acute medical management, manual therapy remains a cornerstone of sustainable rehabilitation. It creates a stronger therapeutic alliance and allows for the integration of active movement during release.
Addressing Musculoskeletal Pain and Referred Patterns
The most deceptive aspect of myofascial pain is referral. The brain, in its attempt to map internal distress, often projects pain to a distant location. This phenomenon makes diagnostic accuracy difficult for those untrained in myofascial maps.
Consider the sternocleidomastoid (SCM). A trigger point here rarely causes pain in the neck. Instead, it refers pain deep into the ear or behind the eye. A patient might see a neurologist for headaches when the root cause is a postural overload of the SCM. Similarly, the infraspinatus is a notorious trickster, frequently responsible for "deep joint pain" in the shoulder that mimics radiculopathy.
Understanding these maps is essential for relief. If we chase the pain, we miss the source. By mapping the referred pain back to its muscular origin, we view musculoskeletal pain not as a localized event, but as a systemic narrative told by the nervous system.
Clinical Reasoning in Treatment Plans
Randomly pressing on sore spots is not a strategy. A robust clinical approach requires a structured protocol.
- Assessment and History
Trigger points are symptoms of overload. If we release the trigger but fail to address the postural slump or leg length discrepancy that created it, the point will return. We must identify the maintaining factors. - Precise Palpation
We use pincer palpation for muscles that can be lifted and flat palpation for muscles against bone. The pressure must be calibrated. Too heavy, and the muscle engages a protective guarding reflex, shielding the trigger point from our work. - The Release Technique
We apply pressure to the barrier of resistance and wait. As the tissue yields, we follow it deeper. This phase is about communicating with the nervous system to downregulate the gamma motor neuron activity that keeps the muscle spindle tight. - Post-Treatment Protocol
A muscle that has been locked in a shortened state is neurologically confused. After release, we must re-educate the tissue through passive stretching followed by active range of motion.
Incorporating Trigger Point Therapy into Rehab
The release is only the beginning. To ensure lasting results, we must bridge the gap between passive treatment and active rehabilitation. This is where incorporating trigger point therapy into a broader movement philosophy is vital.
Once a trigger point is deactivated, the muscle is capable of achieving its full resting length, but the brain still holds a "habit" of limited movement. We must overwrite this. Immediately following manual therapy, I guide the patient through active mobility drills. If we treated the calves, we perform eccentric heel drops. If we treated the pectorals, we move into wall angels.
The nervous system needs to experience the new range of motion without pain to "save" the changes. The benefits of this combined approach – manual release plus active loading – are documented in research showing longer remission periods for chronic pain sufferers.
The Role of Integrative Care
At RSM International Academy, we emphasize that no modality exists in a vacuum. Integrative care means recognizing that a trigger point might be secondary to a lumbar subluxation or systemic inflammation.
We teach our students to recognize the "red flags" that indicate pain is not myofascial. Night pain, unremitting pain, or systemic signs like fever indicate medical pathology. Knowing when not to treat is as important as knowing how to treat. However, for the vast majority of musculoskeletal pain presentations, the myofascial component is significant. Even in osteoarthritis, much of the pain comes from the surrounding muscles splinting the joint. Releasing these trigger points can significantly reduce pain scores.
Myofascial Release vs. Trigger Point Therapy
There is often confusion between general myofascial release (MFR) and trigger point therapy. While they are cousins, they are distinct. MFR typically focuses on broad fascial planes, using shearing forces to separate adhesions. It is a slow, wide-lens approach.
Trigger point therapy is a telephoto lens. It zooms in on specific neuromuscular dysfunction. In practice, I use them sequentially. I use broad myofascial release to desensitize the superficial fascia, allowing access to the deeper musculature where the trigger points reside. Using them together allows for a more profound release. If the fascial casing is tight, the muscle inside cannot relax. Conversely, if the muscle is contracted into a trigger point, it pulls on the fascial casing. You cannot truly treat one without the other.
The Nuance of "The Point"
When we speak of a "point," we risk simplifying the anatomy. It is rarely a single geometric dot. It is often a cluster, a zone of dysfunction. In the gluteals, a spray of trigger points can mimic sciatica in a condition we call "pseudosciatica." The piriformis and gluteus minimus can all refer pain down the posterior leg.
Treating this region requires a 3D understanding of the pelvis. We must sink through the gluteus maximus to access the deeper rotators. This depth of practice is what we cultivate in our Trigger Point Therapy Course. We move beyond charts into the tactile reality of human tissue, exploring how to engage the myofascial system using body weight and leverage rather than brute force.
Elevating Your Practice
For the professional therapist, the addition of advanced trigger point protocols is transformative. It changes the conversation with the patient. You are no longer just managing their discomfort; you are explaining it. You are drawing the lines between their headache and their shoulder tension.
This educational component empowers the patients. When they understand that their pain is a referral from a treatable muscle knot, fear diminishes. They become active participants in their recovery, compliant with the stretching and strengthening exercises necessary to keep the trigger points at bay.
At RSM, we view this work as a blend of rigorous science and intuitive art. The science provides the map – the referral patterns, the chemistry of the sarcomere. The art provides the navigation – the ability to feel the subtle resistance in the tissue.
We invite you to deepen your understanding of this vital modality. Whether you are looking to refine your existing skills or build a new foundation for your clinical practice, mastery of the myofascial system is essential. It is the missing link in many treatment plans and often the key to unlocking chronic, recalcitrant pain.
By integrating these specific, high-level protocols, we do not just treat muscles. We restore the capacity for movement. We resolve the energy crisis that keeps the body in a state of alarm. We turn down the noise of pain so that the patient can return to the life they wish to lead. This is the ultimate goal of our work, and it begins with the skilled application of the hands on the human form.
Shiatsu Massage for Joint Flexibility
The restriction of a joint is rarely a simple matter of shortened muscle fibers. In my years practicing and teaching sports medicine, I have observed that limited range of motion is a complex interplay between neural guarding, fascial densification, and synovial stagnation. Traditional stretching often fails because it addresses the symptom of tightness rather than the neurological and structural drivers of that tightness. This is where the application of manual pressure through the Japanese modality of shiatsu becomes an essential tool for the modern clinician.
During my studies in sports medicine, I became fascinated by how specific, perpendicular compression could alter the state of the autonomic nervous system. Unlike the sliding strokes of Western massage, this approach utilizes a static, penetrating force that communicates directly with the mechanoreceptors embedded in the joint capsule. When we talk about improving mobility, we are really talking about recalibrating the internal sensors that dictate how much movement the brain deems safe.
Integrating Massage and Shiatsu Techniques for Progressive Mobility
A sophisticated approach to physical rehabilitation requires a departure from the idea that more force equals more change. In RSM’s Shiatsu massage training, we emphasize that the efficacy of a treatment lies in its precision. When applying shiatsu techniques, the practitioner utilizes their body weight to create a deep, resonant stimulus. This bypasses the superficial “fight or flight” response, allowing the therapist to reach deeper layers without triggering protective tensing.
The focus on progressive mobility through compression is grounded in the way the body responds to tactile input. By holding a point of tension, we allow interstitial fluid to redistribute within the fascial matrix, creating a “sponge effect” vital for restoring glide between adhered tissue layers. As the tissue softens, the joint is afforded a greater degree of freedom, not through forceful stretching, but through the removal of internal friction.
Experienced massage therapists often find that integrating these rhythmic compressions offers a sustainable way to work. Using the weight of the torso rather than just the strength of the hands allows for a deeper impact with less fatigue. This mechanical advantage is central to our school’s philosophy; we believe the longevity of the practitioner is just as important as the recovery of the patient.
The Biological Logic of a Shiatsu Session
When we structure a shiatsu session, we are following a map that is both anatomical and energetic. While traditional meridians provide a historical framework, the modern sports medicine professional views these as myofascial pathways. A restriction in the ankle is rarely isolated; it is a node in a longer line of tension. The methodology relies on the quality of contact, and waiting for the “unwinding” sensation in the tissue.
This process facilitates a shift to the parasympathetic nervous system, a prerequisite for structural realignment. The specific benefits of this modality include:
- Reduction of Neural Guarding: Deep pressure inhibits overactive muscle spindles, releasing chronic tension.
- Enhanced Circulation: Rhythmic compression encourages the movement of lymph and synovial fluid.
- Proprioceptive Reset: Stimulating the Golgi tendon organs resets the resting length of muscles.
Beyond physiological changes, the practice fosters somatic awareness. Patients often report feeling “more in their body,” an improved body map that is invaluable for injury prevention in high-performance settings.
Clinical Benefits of Shiatsu for Arthritis and Joint Mobility
Managing chronic pain conditions like arthritis requires a delicate balance. Aggressive manipulation can exacerbate inflammation, while inactivity leads to stiffness. Shiatsu massage offers a gentle middle path. By focusing on soft tissues surrounding an arthritic joint, we reduce the mechanical load on articular surfaces, significantly improving joint mobility without aggravating the condition.
In physical therapy, we often see nervous systems sensitized to perceive movement as a threat. The slow cadence of shiatsu provides a safe stimulus, desensitizing these neural pathways. We are teaching the nervous system that pressure does not equal pain. This neurological re-education allows the patient to reclaim their ability to move with ease.
While some bodywork focuses on the muscle belly, our approach considers the joint as the center of the movement experience. We look at the space between the bones. If that space is compromised by tight tendons, the joint cannot function. Through specific pressure on key points, we encourage the limb to “open,” creating a sense of lightness difficult to achieve through other means.
Mastering Pressure and Thumb Placement
Technical precision involves understanding the geometry of the human frame. When I teach, I emphasize that the angle of the thumb is as important as the weight applied. A perpendicular approach ensures force travels directly into the target tissue rather than sliding. This is particularly important near tendon attachments where tissue is dense.
We teach a method of “stacked joints,” where pressure comes from the center of the body and transmits through a straight line of bone. This protects the practitioners and delivers a clear signal to the patient. Effective treatment also involves circulation; compressing and releasing vessels creates a “flushing” effect, bringing oxygenated blood to ischemic areas and clearing inflammatory byproducts.
The Intersection of Tradition and Sports Science
At RSM, we see a synergy between traditional Japanese roots and modern sports science. The concept of energy flow is often viewed with skepticism, yet when viewed through hemodynamics and nerve conduction, the gap closes. A block in flow is often a physical compression. By addressing these physical realities, we restore the body’s capacity for self-regulation.
As the demand for specialized services grows, massage therapy must evolve. The modern patient seeks expertise that goes beyond relaxation. By mastering the nuances of pressure and joint mechanics, we offer care that stands apart. The restoration of flexibility is a collaborative process. When we apply these techniques correctly, we influence the very fabric of the human experience, creating a body that is as resilient and capable as it was meant to be.
Remedial Massage Course Requirements
The transition from general relaxation therapy to clinical intervention marks a definitive threshold in a professional practitioner’s career. It is the moment where the focus shifts from the superficial manipulation of soft tissue to a sophisticated understanding of the kinetic chain, nerve pathways, and postural compensations. At RSM International Academy in Chiang Mai, we recognize that the elite massage therapist does not merely treat a site of pain but identifies the systemic dysfunction that created it.
This requires a shift in perspective from a manual laborer to a clinical thinker who understands the nuances of health science and the mechanics of human movement. The body functions as an integrated tensegrity structure; a restriction in the thoracic spine inevitably echoes in the lumbar region. To address these issues effectively, a professional needs more than a standard massage diploma; they require a specialized framework for identifying and resolving nerve entrapment and postural distortions.
When I founded RSM, my goal was to bridge the gap between traditional manual techniques and the rigorous standards of sports medicine. Our remedial massage training is structured to provide this bridge, ensuring that every technique applied is grounded in functional anatomy and precise clinical reasoning.
The Evolution of the Modern Massage Therapist
Advancing in the field of manual therapy necessitates a deep engagement with the complexities of chronic pain. While basic techniques focus on increasing local circulation, the remedial specialist must delve into the assessment of Upper and Lower Cross Syndromes. These postural patterns are not merely aesthetic concerns but are the primary drivers of functional scoliosis and nerve entrapment. A massage therapist operating at this level must be capable of distinguishing between a muscular strain and a neurological compression.
The educational path to this level of expertise is rigorous. Many students arriving at our academy are already licensed professionals – physiotherapists, athletic trainers, or yoga instructors – seeking to refine their clinical skills. They realize that standard protocols often fall short when dealing with complex cases like Meralgia Paresthetica or Thoracic Outlet Syndrome. The requirement for success is an analytical mind that looks for the source of the “Double Crush Syndrome,” where a nerve is compressed at two or more points along its path.
Within our program, we emphasize that the primary requirement for a remedial practitioner is the ability to perform a thorough physical assessment. This is not about following a pre-set routine; it is about reasoning. Understanding how an anterior pelvic tilt influences the lateral femoral cutaneous nerve is essential for treating hip pain. Without this knowledge, a practitioner may spend hours working on the hip flexors while the true issue remains a persistent nerve glide restriction.
Integration of Remedial Massage Techniques
The structure of our training is intentional and cumulative. We require participants to complete our 20-hour Deep Tissue Massage Course before beginning the specialized remedial module. The logic is simple: you cannot manipulate a nerve sheath if you cannot effectively navigate the muscle layers above it. This combined framework is essential for mastering the depth of pressure and the sensitivity required to work near major nerve plexuses.
The tuition fee for this comprehensive experience is 16,000 THB. This investment covers the 20 hours of Deep Tissue training and the specialized 6 hours of remedial instruction. We have scheduled the remedial sessions specifically from Monday to Friday, 15:10 to 16:10. This cadence allows students to spend the morning absorbing general anatomical principles, then apply a laser focus to specific pathologies, such as functional kyphosis or frozen shoulder, in the afternoon.
This structure allows for a cumulative learning effect. By the time a student reaches the remedial hour, their hands are warmed up, and they are mentally prepared to tackle the nuances of joint mobilization. Unlike a generic therapy school, we do not offer shortcuts. There are no online components to our manual skills training because you cannot learn the subtle resistance of a nerve sheath through a screen. You must be here, hands-on, feeling the tissue change under your fingertips.
The Science of Massage and Nerve Pathologies
When we discuss the requirements for excellence in this field, we must discuss the neurological component of pain. Much of what is categorized as “muscle pain” is actually the brain’s response to perceived threats to the nervous system. In conditions like Thoracic Outlet Syndrome, the compression of the brachial plexus can cause symptoms ranging from numbness to grip weakness. A massage therapist must understand the anatomy of the scalene muscles and the pectoralis minor to effectively decompress this area.
During our practice sessions, we focus heavily on the thoracic spine and the concept of Functional Scoliosis. Unlike structural scoliosis, which involves bony deformity, functional scoliosis is often driven by unilateral muscle spasms in the Quadratus Lumborum (QL) and spinal erectors. By releasing the unilateral tension pulling the spine out of alignment, a skilled practitioner can significantly reduce curvature and restore mobility.
The same principles apply to the lower kinetic chain. We teach students to view the body as a series of levers and pulleys. If the psoas is hypertonic, it does more than just tilt the pelvis; it creates a compressive force on the lumbar vertebrae and can irritate the femoral nerve. By addressing these imbalances with precise treatments, such as Active Soft Tissue Release (ASTR) and hip joint mobilization, we restore the natural kinetic chain. This level of detail elevates a practitioner’s work from general maintenance to corrective therapy.
Work Placement and Professional Standards
For those looking toward future work placement in high-performance environments, such as sports clinics or rehabilitation centers, these skills are non-negotiable. Employers in the healthcare and athletic sectors are looking for therapists who can document their clinical reasoning. If a therapist can explain that they are mobilizing the cervical facet joints to alleviate a tension headache caused by Accessory Nerve compression, they validate their role as a serious clinician.
Earning a diploma or certificate from RSM is an indication that a therapist has undergone rigorous, science-based training. While our academy-issued certificate is not a government license, it is highly respected in the international community of sports medicine. We encourage all participants to check specific licensing requirements in their home countries, as the legal framework for massage varies globally. However, the skill requirement – the ability to resolve pain – is universal.
The remedial massage practitioner must be a lifelong student. The field of myofascial research is constantly evolving, and the techniques we use today are refined by the latest findings in health science. At RSM, we emphasize the importance of continuous study and the refinement of manual sensitivity. The hand is an assessment tool just as much as it is a tool for treatment.
Ultimately, the goal of these courses is to restore the body to its optimal state of function. This requires a blend of art and science, of intuition and evidence-based practice. By focusing on the underlying causes of pain, such as postural misalignment and nerve compression, we provide a service that is both essential and transformative. Through our specialized skills training, we provide the tools, but the dedication must come from the therapist. Together, we can elevate the profession of massage to new heights of clinical efficacy.
Applying Hydrotherapy in Orthopedic Massage: A Clinical Integration for Recovery
The human integumentary system is a sophisticated biological interface, registering every nuance of thermal and mechanical pressure. In sports medicine, we often view the skin merely as a barrier to bypass to reach underlying myofascial structures. This perspective ignores a fundamental physiological lever. Water possesses a heat capacity and thermal conductivity that far exceed those of air, making it an exceptionally efficient medium for altering physiology. When we integrate these thermal properties into a manual therapy framework, we are engaging the autonomic nervous system to facilitate deeper orthopedic interventions.
At RSM International Academy in Chiang Mai, my approach when teaching the Orthopedic Massage Course is grounded in the reality of the biological response. We do not use thermal modalities simply for relaxation; we use them because they provide a predictable influence on tissue compliance and nociceptive signaling. Hydrotherapy, when applied with precision, acts as a force multiplier. By strategically altering tissue temperature, we can achieve outcomes that would be impossible through mechanical pressure alone.
Thermal Modulation and the Mechanics of Hydrotherapy
The efficacy of water as a therapeutic agent lies in its ability to transfer energy. This energy transfer initiates a cascade of vascular and neural responses. While most clinicians understand basic vasodilation and vasoconstriction, the nuance of how these shifts impact orthopedic massage is often overlooked. We must consider the hypothalamus as the regulator. When a localized area undergoes significant temperature change, the body initiates a reflexive response to maintain homeostasis. We exploit this reflex to influence deep tissue layers our hands cannot directly reach.
Hydrotherapy operates through conduction. When a heated or cooled medium contacts the skin, energy moves along a gradient, progressively saturating the tissue. For the therapist, the timing of this saturation is critical. Applying heat briefly affects only superficial capillary beds, whereas prolonged application reaches deeper fascia, changing the viscosity of interstitial fluid and the extensibility of collagen fibers.
Strategic Use of Warm Hydrotherapy
Integrating warm hydrotherapy into a treatment plan for chronic dysfunction addresses the physical properties of connective tissue. Collagen exhibits thixotropy: in a resting, cooler state, fascial ground substance is gel-like and resistant. Controlled warmth shifts this toward a fluid, sol-like consistency. This transition is essential for conditions like adhesive capsulitis where tissue has become restricted.
Warmth also triggers the gate control theory of pain. Thermal receptors (TRPV1 channels) send signals to the spinal cord that effectively “crowd out” nociceptive signals. When the patient’s perception of pain is dampened by heat, the therapist can employ deeper massage techniques without triggering protective muscle guarding. This synergy between thermal comfort and mechanical intensity is the hallmark of sophisticated care.
Furthermore, as vessels dilate, circulation accelerates, delivering oxygen to the injury site while removing metabolic byproducts. This is particularly relevant for hypertonic muscles trapped in an ischemic cycle. Warmth breaks this cycle by restoring blood flow, allowing muscle fibers to release their sustained contraction.
Clinical Precision in Cold Hydrotherapy
While warmth provides plasticity, cold hydrotherapy offers control, particularly for acute injury and inflammation. The goal is vasoconstriction and reducing metabolic demand. When an athlete suffers a sprain, the primary concern is secondary hypoxic injury – swelling that compresses capillaries and deprives healthy cells of oxygen. By applying cold, we lower the metabolic rate of these cells, allowing them to survive reduced oxygen availability.
Cold hydrotherapy is also valuable in managing localized inflammation following intense manual therapy. Deep transverse friction on a chronic tendinopathy creates controlled micro-trauma. Applying a cold medium afterward contains the inflammatory response, ensuring it remains therapeutic rather than excessive.
We also use cold to address nerve conduction velocity. Lower temperatures slow the speed at which peripheral nerves send signals. For a client with nerve entrapment or spasms, a brief application of ice provides a sedative effect, permitting the therapist to address structural compression without irritating the sensitized nerve.
The Dynamics of Contrast Hydrotherapy
Perhaps the most sophisticated use of thermal energy is contrast hydrotherapy. This technique involves rapid alternation between hot and cold applications, creating a vascular pump. As vessels repeatedly dilate and constrict, they actively move fluid through tissues. For rehabilitating chronic edema or aiding recovery after high-intensity training, this method is remarkably effective.
In practice, ratios are vital. A standard protocol might involve three minutes of heat followed by one minute of cold, repeated several times. Heat provides expansion; cold provides the contraction that drives fluid toward the lymphatic system. This rhythm shifts the autonomic nervous system from a sympathetic “fight or flight” state toward a parasympathetic “rest and digest” state – a critical shift, as the body cannot effectively repair tissue under chronic stress.
In orthopedic contexts like post-surgical knee recovery, contrast work resolves deep-seated swelling that manual drainage alone cannot move. It also serves as a sensory “reset” for the joint, helping to clarify the neural representation of the area and reducing phantom pain sensations.
Practical Integration and Hydrotherapy Tools
Successful integration requires the right hydrotherapy tools and a seamless workflow. We do not want the application of water to be an interruption. The choice of tool depends on the desired depth of penetration and the pathology.
For example, when treating a pitcher’s shoulder, I might use a moist heat pack to soften the capsule before joint mobilizations. Later, I might use an ice cup for ice massage along the infraspinatus to mitigate inflammation. This specificity is what we teach at RSM; it is about matching the modality to the biological need.
Hydrotherapy equipment must be maintained with clinical rigor. Heat packs that are too hot can cause thermal stress; cold packs that are insufficient will fail to elicit vasoconstriction. The professional therapist must be as disciplined with their tools as they are with their manual techniques.
Clinical Considerations for Hydrotherapy Application
To implement these techniques safely, the therapist must adhere to specific guidelines. The following list outlines primary considerations for integrating thermal modalities:
- Thermal Tolerance Assessment: Before any application, verify the client’s ability to perceive temperature. This is critical for clients with diabetes or neuropathy. A simple test with a warm and cool object confirms sensory pathways are intact.
- Tissue Response Monitoring: Monitor the skin throughout the treatment. While erythema is expected with heat, mottling or extreme pallor demands immediate attention. The therapist must remain attentive.
- Contraindication Screening: Conditions like open wounds, cardiac insufficiency, or acute inflammation (for heat) strictly prohibit hydrotherapy.
- Hydration and Systemic Impact: Thermal shifts affect blood pressure. Encourage clients to hydrate before and after sessions. Be aware of orthostatic hypotension when a client stands after heat therapy.
The RSM Philosophy on Fluid Dynamics
At the core of our teaching is the understanding that the body is a fluid-driven machine. Every cell exists in an aqueous environment. When we use hydrotherapy, we are managing the hydraulics of the human frame. This shifts the therapist’s role from manual laborer to biological engineer.
The most successful therapists synthesize information from multiple disciplines. Hydrotherapy bridges the mechanical interventions of massage therapy and the physiological realities of healing. It allows us to work smarter. By letting the thermal properties of water change tissue state, our hands remain sensitive for the precise work only human touch can provide.
In sports medicine, speed of recovery is the metric that matters. Whether for an athlete or a desk worker, the goal is efficient tissue repair. Water therapy allows us to hit those targets consistently, providing a level of control over the healing environment that manual work alone cannot match.
Advanced Protocols and Rehabilitation
As we delve into complex cases, the application becomes more nuanced. In chronic myofascial pain syndrome, trigger points are areas of metabolic distress. A therapist might use a “spray and stretch” technique – a form of hydrotherapy using vapocoolant. The sudden cold distracts the nervous system, allowing a passive stretch that would otherwise be too painful.
Another advanced application is using warm baths for distal extremities. When working on hand or foot joints, direct manual work can be aggravating if tissue is sensitized. Immersion in warm water allows for active-assisted range of motion exercises. The buoyancy reduces joint load while warmth maintains extensibility, a combined approach effective for post-fracture rehabilitation.
We must also consider the psychological component. Pain is an emotional experience. The soothing nature of warm water reduces global stress, lowering cortisol. This systemic relaxation makes the orthopedic massage more effective, as the body is no longer in a defensive posture.
The Future of Integrated Orthopedic Care
The landscape of manual therapy evolves, yet physiological laws remain. The use of water as a healing agent is ancient, but we are only now understanding its full molecular impact. As research advances, our protocols will continue to be refined.
At RSM International Academy, we encourage students to understand the “why” behind every technique. When you apply a heat pack or ice, you initiate a dialogue with the client’s biology. The quality of that dialogue determines the outcome. By mastering hydrotherapy treatments, you expand your clinical vocabulary and provide a sophisticated path to recovery.
The integration of these techniques fulfills the potential of massage. It acknowledges the body as a complex system requiring a multi-faceted approach. I encourage you to see water not just as a tool, but as a partner in the healing process.
The path to expertise involves constant refinement. By bringing hydrotherapy techniques into your clinical work, you choose to work in harmony with physiological processes, facilitating deep healing. This is the essence of the RSM method. Through the careful balance of heat and cold, we unlock the body’s capacity for health, ensuring every client leaves stronger and closer to their goals.
Myofascial Release Courses for Physical Therapists
The anatomical map inherited from the last century of medical science is, in many ways, a deception of the scalpel. When we dissect, we cut through connective tissue to isolate muscle, naming the parts while discarding the medium that binds them. For the clinician responsible for high-performance rehabilitation or complex pathology, this reductionist view is no longer sufficient. We are recognizing that the body is not a collection of levers and pulleys, but a pressurized, continuous system of tension and compression.
This realization demands a shift in how we approach manual therapy. It requires us to look beyond the insertion and origin of muscle fibers to the network that envelops them. At the RSM International Academy, we often observe that even highly qualified professionals arrive with a disjointed understanding of this system. They possess excellent knowledge of the “hardware”, the bones and nerves, yet lack the tactile fluency to engage with the “software.” The fascial network acts as a communicative organ that dictates structural integrity. In RSM’s Myofascial Release Course, students learn that the ability to manipulate this tissue is not an add-on skill; it is the requisite evolution for any therapist seeking to move from symptom management to structural correction.
The Evolution of Myofascial Release in Clinical Practice
The history of manual intervention has been characterized by a migration from aggressive adjustments toward interventions that respect the viscoelastic properties of tissue. Early iterations of fascial work were often predicated on the mechanical concept of “breaking down” adhesions. This phrasing, while common in massage therapy, betrays a misunderstanding of material science. Fascia is stronger than steel by weight; the notion that a human hand could mechanically tear such a dense network through brute force is physiologically inaccurate.
Contemporary practice focuses instead on mechanotransduction – the cellular process by which physical load is converted into biochemical signals. When a therapist applies sustained, vector-specific pressure, they are signaling the fibroblasts within the extracellular matrix to alter their production of collagen. This process requires a patience often absent in high-volume clinical settings. It distinguishes the act of forcing a tissue from the art of communicating with it.
By engaging the tissue at its inherent rhythm, the therapist induces a state of “creep,” allowing fibers to realign and ground substance to rehydrate. This is why the study of myofascial release is critical for those in rehabilitative sciences. It provides a toolkit for addressing global patterns of tension that underlie local symptoms. A clinician might treat a hamstring strain repeatedly with limited success because they fail to address a restriction in the thoracolumbar fascia. High-level education allows the practitioner to visualize and treat these longitudinal relationships.
Deep Tissue Mechanics and the Myofascial Layer
To effectively intervene, one must possess a granular understanding of the body’s stratification. The myofascial layer is not a monolith; it is a complex laminate structure where depth determines function. There is a profound difference between manipulating the superficial fascia, which houses a dense network of cutaneous nerves, and the deep fascia, which compartmentalizes muscle groups.
The superficial layers are highly responsive to light, shearing touch, primarily interfacing with the autonomic nervous system to down-regulate sympathetic tone. If a therapist plunges too deep too quickly, they trigger a defensive stiffening, rendering deep work impossible. The deep investing fascia, conversely, is designed for load transmission. Here, the clinical objective is to restore the sliding surfaces between muscles. In a healthy state, the epimysium should glide frictionless against its neighbor. In pathological states, this lubricant densifies.
When observing a master clinician, it may appear they are doing very little. In reality, they are using palpation to locate the precise vector of densification and waiting for the tissue to undergo a phase change. This level of manual precision separates the elite practitioner from the novice.
Addressing Chronic Myofascial Pain Through Manual Load
The clinical presentation of myofascial pain is rarely a localized event. It is almost always the result of a systemic failure to distribute load efficiently. When a specific segment of the kinetic chain loses mobility, force is shunted to adjacent structures, eventually causing them to fail. This manifests as the familiar “knot,” but treating only the site of pain is akin to silencing a fire alarm while the building burns.
A sophisticated assessment protocol traces these lines of tension back to their silent origins. We frequently find that the painful tissue is merely the “victim,” while the “criminal” is an asymptomatic restriction located elsewhere. For instance, chronic suboccipital tension is often a compensatory strategy for a restricted rib cage. Without a holistic map of these connective tissue pathways, the therapist is condemned to chase symptoms indefinitely.
The application of specific techniques serves a dual purpose: mechanically encouraging tissue remodeling and neurologically providing potent sensory input to the central nervous system. Chronic pain often leads to “cortical smudging,” where the brain’s representation of a body part becomes blurry. Precise manual intervention provides a high-fidelity signal that assists the brain in regaining accurate motor control.
Navigating Advanced Courses and Skill Acquisition
The marketplace for professional development is saturated, yet few courses offer the depth required by a seasoned medical professional. For a physiotherapist or sports medicine doctor, a weekend workshop covering basic strokes is insufficient. These professionals require a rigorous framework that integrates seamlessly with their existing knowledge of biomechanics and pathology.
When selecting continuing education, the pedagogical approach is paramount. A high-quality program must do more than demonstrate where to place one’s hands; it must teach the student how to think three-dimensionally. It must bridge the gap between emerging research in fascial science and the tactile reality of the treatment room. This necessitates a deep dive into the neurophysiology of touch, fluid dynamics, and biotensegrity.
There is a disturbing trend in the industry attempting to migrate these courses to online platforms. While digital resources are excellent for theoretical review, the tactile nuance required for deep tissue manipulation evaporates on a screen. You cannot learn to feel the density of a trigger point or the viscosity of hyaluronic acid through a video module. The manual aspect requires a lab environment where a master teacher can palpate the student’s work, correcting pressure and intention in real-time. There is no substitute for this feedback loop.
The RSM Philosophy: Science Meets Intuition
I founded RSM International Academy to bridge a specific gap in the medical community. My background in sports medicine instilled in me a reverence for data and objective measurement. Yet, my decades at the treatment table taught me that the human body possesses a wisdom that often defies linear logic.
We frequently encounter students searching for myofascial release seminars that promise a quick fix. I am compelled to tell them that no such protocol exists. What exists is a refined capacity for listening. When we teach release techniques, we are teaching a form of non-verbal dialogue. We are training the therapist to detect the subtle variations in temperature and “give” that signal a successful intervention.
This is why we place such immense weight on the hands-on component of our training in Chiang Mai. One can read every paper on the myofascial trigger, but until you have felt one dissipate under your fingers, the knowledge remains abstract. The trigger is often merely the loud symptom of a quiet systemic problem. We believe that a certificate should represent more than attendance; it should signify a fundamental shift in the therapist’s ability to perceive the human form.
The integration of these skills into a sports medicine context is particularly potent. In elite athletics, a one-percent improvement in mobility or recovery speed can determine a career trajectory. Myofascial work provides that edge by ensuring the athlete’s structural system operates without internal friction.
The Future of Manual Intervention
The landscape of physical therapy is undergoing a necessary renovation, moving toward a model that recognizes the inextricable link between structure and psyche. In this emerging paradigm, the therapist is not a mechanic repairing a broken part but a facilitator of the body’s innate homeostatic drive.
High-quality seminars are now incorporating elements of neuroscience and complex systems theory. We are learning that the state of the therapist’s own nervous system is a clinical variable. If the practitioner is stressed or distracted, the patient’s fascia will sense that tension and remain guarded. The work, therefore, begins with the therapist’s own self-regulation.
When a physical therapist chooses to specialize in this field, they are choosing to master one of the most complex aspects of human healthcare. It is a path that demands intellectual rigor and physical discipline. The rewards, however, are profound. There is deep satisfaction in assisting a patient who has exhausted standard medical options, finally finding relief through a nuanced understanding of their connective tissue.
In our academy, we do not simply teach a modality; we cultivate a mindset. We aim for our graduates to become the clinicians other doctors consult when a case proves intractable. By focusing on the intersection of sports medicine science and the art of myofascial release, we provide a pathway to that level of excellence. The fascial system is the great unifier of human anatomy. Mastering its language of tension and fluidity is the key to unlocking the full potential of your clinical practice.
Keeping Massage Techniques Up to Date: A Science-Based Approach
Stagnation in Clinical Practice
A therapist can spend decades refining a specific sequence, mastering the rhythm until it feels like a biological truth. Yet, without a rigorous commitment to evolving that practice, proficiency calcifies into stagnation. The human body is not a static object, and our understanding of its mechanics changes with every major publication in physiology and neuroscience. To rely solely on the anatomical maps of twenty years ago is to treat a version of the human body that science has largely left behind.
At RSM International Academy, during our courses and workshops in Chiang Mai, we teach from the cutting edge of sports medicine insights, and instill the value of continual learning.
The Evolution of Massage Therapy
We must acknowledge that the massage profession has historically struggled with a dichotomy between intuition and evidence. On one side lies the weight of ancient tradition; on the other, the reductionist rigour of Western medicine. Our work exists in the friction between these worlds. It is no longer sufficient to treat a muscle simply because it feels tight. We now understand that hypertonicity is often a neurological defense mechanism.
When a massage therapist applies force to a “knot,” they are not physically breaking down adhesions; they are communicating with the nervous system. They are providing sensory input to modulate gamma motor neuron activity. If we believe we are physically reshaping tissue, we might use excessive force that causes protective guarding. If we understand we are modulating neural input, our approach becomes more subtle and effective.
Why Traditional Techniques Must Adapt
There is a profound respect for heritage in our industry, yet traditional techniques must be scrutinized through modern physiology. Consider the concept of “flushing” lactic acid. For decades, it was taught that vigorous effleurage removed metabolic waste. We now know that active recovery is significantly more effective.
Does this mean the technique is useless? No. It means the justification must change. We are not flushing toxins; we are modulating the parasympathetic nervous system to optimize recovery. When we update our theoretical framework, we inevitably update our manual application. We stop chasing myths and start targeting physiological realities.
The Educational Gap: Beyond the Basic Certificate
A primary driver of stagnation is foundational education. The average massage school operates on a curriculum designed for entry-level competency, not mastery. They teach students how to pass a licensing exam, often involving memorized anatomy that varies in real life. When a student graduates and receives their certificate, they often believe they are finished learning. In reality, they have merely been given a license to start.
The gap between standard massage training and elite sports medicine is vast. In a standard program, you might learn to rub a sore hamstring. In advanced therapy training, you learn to assess whether that hamstring pain is a local strain, a referential pattern from the lumbar spine, or protective tension from pelvic instability. Massage schools must evolve to include differential diagnosis, but until then, it is the therapist’s responsibility to seek higher education.
The Responsibilities of the Elite Massage Therapist
The modern practitioner must be a lifelong researcher. The massage therapist working with athletes cannot afford to be passive. We see this clearly in how we treat tendinopathies. Historically, deep transverse friction was the gold standard to break down scar tissue. Current research suggests that while friction has analgesic effects, the mechanical load required to remodel collagen is greater than human hands can provide.
The focus has shifted toward loading protocols and neuro-modulatory soft tissue work. If a therapist is not reading current literature, they might be grinding away at a tendon, causing pain without structural change. The massage industry must move toward a model where continuous learning is a requirement for licensure, not an optional hobby.
Continuing Education as a Clinical Necessity
Continuing education is often viewed as a box to tick. At RSM, we view it as fuel for clinical intuition. Intuition is the subconscious processing of data; the more high-quality data you feed your brain through advanced training, the more accurate your intuition becomes.
When we study the body in a dissection lab, we see the continuity of fascia. We see the latissimus dorsi is not an isolated triangle of meat but a structure connected to the gluteus maximus via the thoracolumbar fascia. This transforms how we treat lower back pain; we stop looking at the lumbar erectors in isolation and assess contralateral shoulder function. Basic massage schools rarely cover this connectivity, teaching muscles as discrete units. Updating your knowledge means moving to a global, functional view.
Analyzing the Latest Massage Research
To truly innovate, one must look at what the latest massage research says about mechanotransduction: how cells convert mechanical stimulus into chemical activity. When we apply pressure, we are altering the chemical environment of the tissue.
Recent studies on the extracellular matrix suggest that specific shearing forces can influence hydration and sliding potential between fascial layers. We now know we cannot “stretch” fascia like a rubber band, because it is too strong. However, we can hydrate it to improve glide. This changes the intent of the massage. We work to restore sliding surfaces to prevent nerve entrapment, often the true source of pain in conditions like carpal tunnel.
Key Shifts in Modern Manual Therapy
- From Structural to Functional: A symmetrical skeleton is less important than a pain-free range of motion.
- From Operator to Interactor: The therapist interacts with a living ecosystem. The patient’s nervous system determines if a muscle relaxes.
- From Pain as Damage to Pain as Output: We treat the threat level, not just the tissue pathology.
Advanced Training for Complex Rehabilitation
The bridge between a spa treatment and medical massage therapy is assessment. In our training modules, we emphasize that 60% of the treatment happens before the client gets on the table. Massage techniques are merely tools; intelligence lies in selecting the right one.
Treating a marathon runner two days before a race requires a different protocol than treating them two days after. Pre-event work maintains neural tone; post-event work focuses on down-regulation. Many therapists struggle with this nuance, applying a cookie-cutter “sports massage” to every athlete. Modern wellness demands specificity regarding the sport, training cycle, and injury history.
The Role of Science in Soft Tissue Work
There is growing demand for medical integration. Doctors are open to collaboration if therapists speak their language. When a therapist explains a treatment plan in terms of physiological outcomes rather than energy flow, they gain credibility.
We must demonstrate that our work is reproducible and grounded in science. This involves understanding concussion management, pharmacological contraindications, and red flags. Furthermore, we must embrace the biopsychosocial model. The therapeutic alliance is a significant pain modulator. Science confirms that a patient who feels heard experiences better outcomes, elevating communication skills to the level of manual skills.
Integrating New Findings into Daily Practice
Integrating knowledge requires disrupting habit. I challenge students to audit their practice: “Why do you do that move? Is there a more efficient way?” If the answer is “because I was taught that way,” it is time to dig deeper.
Consider the iliotibial (IT) band. For years, therapists rolled it aggressively. We now know the IT band is a thickening of fascia designed for stability, not a muscle. Crushing it causes pain, not length. The modern approach targets the tensor fasciae latae and gluteus maximus; the muscles tensioning the band. We treat the engine, not the cable. Effective massage often innovates through subtraction – removing ineffective elements to focus on what influences the nervous system.
The Future of Manual Therapy
The future belongs to the hybrid practitioner. The boundaries between yoga, physical therapy, and massage are blurring. We see massage techniques integrated into movement classes, and movement assessments in massage sessions. This convergence is driven by a holistic understanding of health.
At RSM, we encourage students to look outside the silo of “bodywork.” Study gait mechanics and orthopedics. Build a dynamic mental map of the human body. When a client presents with plantar fasciitis, we look at calf flexibility, pelvic tilt, and breath mechanics. This detective work keeps the profession intellectually stimulating.
Redefining the Therapeutic Relationship
Keeping up to date involves rethinking the therapeutic relationship. The new model is collaborative, empowering clients with education. When a client understands the mechanism of their injury, compliance with rehabilitation improves. They become partners in their recovery. This shifts the locus of control to the patient, a key factor in long-term health outcomes.
The pursuit of knowledge is an infinite game. In the high-stakes world of sports medicine, constant refinement is the standard. The body evolves, science evolves, and so must we.
The Intersection of Biology and Mechanics
To understand the muscle is to understand our history. We are designed for locomotion, yet modern lifestyles impose static loads, creating pathologies like “tech neck.” Treating these requires understanding ergonomics. A massage therapist who understands biomechanics can offer advice on workstation setup, moving from palliative to curative care.
We must also consider the biochemical environment. Inflammation is the first stage of healing. Suppressing it indiscriminately can delay repair. Manual therapy can assist in resolution by improving fluid exchange, but timing is critical. Applying deep pressure during acute inflammation can cause damage. Knowing when not to touch is as important as knowing how to touch.
The Path Forward
The path to excellence is paved with curiosity. Whether working in a spa or a locker room, the principles remain the same. We founded RSM International Academy to serve those unsatisfied with the status quo. We believe massage is a sophisticated form of healthcare deserving rigorous academic backing.
By staying current with literature and questioning our methods, we honor the trust our clients place in us. The stagnation trap is easy to escape; it requires opening a book or stepping back into the classroom. The science of the human body is the most fascinating subject on earth. As long as we keep learning, we keep our practice alive.
Dry Needling vs Trigger Point Massage: Efficacy and Mechanism
There is an unmistakable texture to a dysfunctional muscle belly. It presents as a dense physiological snag in the body’s kinetic fabric. To the patient, this is a source of referred pain and restricted motion; to the practitioner, it is a riddle. The fundamental question in modern manual medicine is not whether these trigger points exist, but which tool is superior for unraveling them: the invasive precision of dry needling, or the ischemic pressure of the human hand.
In RSM’s Trigger Point Therapy Course, we teach that the choice of modality dictates the physiological response. While both treatments target the same pathology, their mechanisms are distinct. Understanding this divergence is critical for the serious therapist.
Trigger Points and The Mechanism of Action in Dry Needling
To evaluate the tool, we must understand the target. A myofascial trigger point is a localized area of hypoxia. Dysfunctional motor endplates release excessive acetylcholine, locking sarcomeres into a state of perpetual contraction. This creates a “tight band” of muscle tension that strangles local capillaries, preventing the muscle from flushing out metabolic waste.
Dry needling, a technique widely adopted by physical therapists and sports physicians, addresses this via mechanical disruption. It is termed “dry” to distinguish it from trigger point injections, where medication is delivered via hypodermic needle. Here, the filament needle itself is the agent of change.
When a needle penetrates the trigger, it creates a micro-lesion. This invasive stimulus typically elicits a “local twitch response,” a spinal reflex where the muscle fibers involuntarily contract and then release. This twitch is the clinical gold standard of a successful needling session. It signifies a rapid depolarization that resets the muscle spindle, restoring normal length-tension relationships.
The primary virtue of needling is depth. Anatomical structures like the deep multifidus or the subscapularis are mechanically difficult to isolate with manual pressure alone. A needle bypasses superficial layers to strike a deep trigger with absolute precision, offering relief for chronic, calcified trigger points that have resisted conventional stretching.
Trigger Point Massage Therapy as a Diagnostic Tool
However, precision is not the only metric of success in therapy. While a needle is an exceptional tool for disruption, it is a poor tool for diagnosis. A needle cannot feel; it provides no sensory feedback until it strikes a structure.
In contrast, massage therapy is inherently diagnostic. The human hand serves as a listening device. Through palpation, we detect subtle changes in tissue texture, temperature, and hydration that a needle would miss. Trigger point manual work operates on the principle of “ischemic compression.” By applying sustained pressure, the therapist temporarily occludes blood flow. Upon release, the body responds with reactive hyperemia: a rush of fresh, oxygenated blood that flushes out inflammatory cytokines.
This approach treats the myofascial network as a continuum rather than a series of isolated points. A trigger in the upper trapezius is rarely a solitary event; it is usually part of a tension chain involving the neck and pectorals. Manual therapy allows the practitioner to address this entire kinetic chain, stripping fascia and stretching fibers in ways a needle cannot.
The Role of Point Therapy in Pain Management
When comparing dry needling against manual techniques, studies suggest they serve different phases of rehabilitation. Dry needling is often superior for the “reset” – the immediate pain relief and restoration of range of motion in stubborn holding patterns. It is a shock to the system that breaks the cycle of dysfunction.
Manual therapy, however, is often better suited for maintenance and stress reduction. Needling is a sympathetic stressor; it can be painful and leave the muscle feeling bruised. Manual work induces a parasympathetic response, lowering cortisol and encouraging relaxation. For a patient with central sensitization or a fear of injections, the aggressive nature of a needling trigger approach may be counterproductive, whereas the broader input of massage is safe and effective.
Physical Therapists Scope of Practice
The distinction is also legal. In most regions, dry needling is restricted to licensed physical therapists, doctors, and acupuncture practitioners due to the need for advanced neuroanatomical knowledge.
However, this limitation invites mastery. At RSM, we emphasize that a skilled manual therapist can achieve results comparable to needling by understanding referral patterns. For physical therapists who do use needles, the danger lies in reliance. The needle releases the trigger, but it does not re-educate the movement pattern that caused the injuries or dysfunction.
Effective physical therapy must integrate the release with neuromuscular re-education. Ultimately, the debate is not about which tool is better, but when to apply each. Needling offers mechanical advantage; manual work offers sensory connection. The most sophisticated practitioners utilize the philosophy of both, understanding that healing requires not just the release of the trigger, but the restoration of the body’s functional harmony.
Shiatsu Massage for Immune Support: The Physiology of Defense
The human body is under constant, invisible siege. Every day, we navigate a microscopic battlefield of pathogens, environmental toxins, and the silent accumulation of physiological stress. At RSM International Academy, we often encounter students and patients who view immunity as a nebulous force; something to be “boosted” with a supplement. But to the trained eye of a sports medicine specialist, immunity is a tangible, mechanical reality. It is a function of flow, neural balance, and cellular readiness.
In RSM’s Deep Shiatsu Massage Course we teach much more than relaxation, we teach sports-medicine-informed manual interventions that interface with the autonomic nervous system to strengthen the body’s innate capacity for defense.
The Impact of Massage Therapy
To understand how manual therapy influences the body, we must first understand what compromises it. In my experience treating high-performance athletes, the primary antagonist to a healthy immune system is chronic sympathetic dominance.
When a client enters a state of high stress, whether from overtraining or daily life, their body floods with cortisol. In the long term, cortisol acts as a potent immunosuppressant, inhibiting the activity of Natural Killer (NK) cells, the body’s frontline sentinels.
This is where the precision of massage therapy becomes a clinical tool rather than a luxury service. Unlike modalities that focus solely on circulatory flow, shiatsu utilizes perpendicular pressure that penetrates deep into the muscle belly. This stimulation triggers a specific parasympathetic response, mechanically downregulating the “fight or flight” mode. We are effectively issuing an “all clear” signal, allowing the body to divert resources from survival back to repair.
Shiatsu Massage and Cellular Defense
The link between manual therapy and immune resilience is well-documented in clinical literature. Research has consistently shown that manual therapy can lead to measurable increases in the activity of lymphocytes. At our center in Chiang Mai, we emphasize to our students that the skin is an external nervous system.
When we apply the sustained, rhythmic pressure characteristic of shiatsu massage, we are stimulating the vagus nerve. This stimulation does more than slow the heart rate; it enhances the cytotoxicity of immune cells. In sports medicine, we understand this as “host optimization.” We cannot control the pathogen, but we can control the host’s terrain. A body returned to parasympathetic balance through skilled shiatsu sessions is a fortress secured.
Japanese Massage and Anatomical Pathways
While Western medicine frames immunity in terms of white blood cells, Traditional Chinese and Japanese massage speaks of “Wei Qi” (Defensive Energy). For the skeptical scientific mind, these concepts can initially seem abstract. However, we train our students to see the anatomical correlates behind these ancient maps.
The body meridians used in Shiatsu often trace pathways that mirror significant neurovascular bundles. By treating specific points, we influence the structures governing respiratory and lymphatic health:
- LU-1 (Zhongfu): Located in the first intercostal space, this point sits near the lymphatic nodes of the axilla. Releasing tension here improves thoracic mobility, allowing for deeper respiration.
- LU-7 (Lieque): Found near the wrist, stimulation here influences the radial nerve, affecting tension patterns in the neck that can contribute to headaches.
- ST-36 (Zusanli): Located on the tibialis anterior, stimulation of this point links to increased gastric motility and systemic regulation.
Deep Techniques to Support Immune Function
Effective shiatsu therapy is not about brute force; it is about depth. To achieve the deep physiological changes required for modulation, the practitioner must sink into the tissues. This approach provides profound relief from the muscular armor that chronic stress builds.
When the intercostal muscles are rigid, breathing is shallow and lymphatic drainage is impeded. By releasing these restrictions, shiatsu helps physically unclog the body’s filtration systems. We also address the “sickness behavior” loop. By flooding the system with sensory input that signals safety, we allow the patient to rest deeply. It is in deep sleep, facilitated by this support, that the body does its most heavy lifting.
The RSM Standard of Care
At RSM International Academy, we believe that providing immunity massage requires a sophisticated understanding of pathology. It is not enough to rub the skin; one must understand what lies beneath it.
Whether you are a physiotherapist or a wellness professional, integrating these techniques offers a powerful adjunct to standard care. The benefits extend beyond the session, offering clients improved sleep and greater resilience. This is the essence of true services in sports medicine: empowering the body to do what it was designed to do, only better. By mastering the art of massage, we offer our clients a vital layer of protection – one built from the inside out.
Adapting Orthopedic Massage for Children: What Every Practitioner Needs to Know
Picture a typical scenario: a child on a treatment table, swinging their legs, fidgeting with their socks. A parent hovers near the door, visibly anxious. The child is not anxious at all; they are bored. They want to go back outside. Anyone who has worked with young patients recognizes this scene instantly. The tissue is different, the psychology is different, and the clinical reasoning that serves you well with adults will, if applied without modification, fail you entirely.
At RSM International Academy, I emphasize that a child is not a small adult. The musculoskeletal system of a growing child presents distinct anatomical characteristics that demand a different approach to manual therapy. The bones are less dense, more porous, and still actively undergoing ossification. Growth plates (physes), composed of hyaline cartilage, sit at the ends of long bones and remain open until the mid-to-late teenage years. These structures are among the weakest links in the child’s musculoskeletal chain, more vulnerable to injury than the surrounding tendons and ligaments.
Why Massage Techniques Require Structural Awareness
In adult orthopedic massage, a therapist can apply sustained deep pressure along a muscle belly or mobilize scar tissue with confidence that the underlying bone is fully mineralized. In children, each of these decisions must be reconsidered. Bone density is lower, the periosteum is thicker and more biologically active, and the epiphyses may be partially or entirely composed of cartilage. Physeal injuries account for approximately 15 to 18 percent of all fractures in children. A practitioner working near the knee, wrist, or ankle must understand that excessive mechanical stress at or near a growth plate can interfere with normal bone development.
This does not mean that massage is contraindicated in children. It means that pressure, direction, and location of force all need to be calibrated with an awareness of developmental anatomy.
Adapting Pressure and Pacing in Therapy for Young Athletes
Pressure modulation is the single most important variable when transitioning from adult to pediatric bodywork. Research on massage for children consistently shows that moderate pressure produces the most favorable outcomes, while light-pressure massage tends to produce an arousing rather than calming effect. The therapeutic window is narrower than in adults, and the consequences of overshooting it are both physiological and psychological.
In RSM's Orthopedic Massage Course, I teach my students to think of pressure as a conversation with the tissue. With a child, that conversation includes a nerve system that may be less capable of articulating discomfort, connective tissue that is more hydrated and elastic, and bone that is still hardening. Sessions should be shorter; twenty minutes is a common benchmark, and child massage sessions that run too long risk overstimulation.
Managing Post-Injury Rehabilitation Through Hands-On Care
Children involved in organized sports sustain soft tissue injuries at rates comparable to adults, but the healing timeline is shaped by growth. The rehabilitation journey for a young athlete recovering from an Osgood-Schlatter or Sever’s disease presentation is defined by the fact that the apophysis is still maturing. Aggressive mobilization near these sites could aggravate an already irritated growth center. The therapeutic goal is to reduce tension in the surrounding musculature, improve local circulation, and support the body’s own recovery mechanisms.
A practical approach to post-injury care includes:
- Gentle effleurage and petrissage applied proximal to the injury site, avoiding direct pressure on apophyseal or epiphyseal structures.
- Myofascial release at slow velocity and low load, respecting the higher elasticity of children’s connective tissue.
- Active engagement of the child through breathing cues, movement requests, and verbal check-ins to maintain trust and assess pain tolerance.
Working with Cerebral Palsy and Muscle Tone Disorders
Massage therapy for children extends well beyond sports-related injury. Research has documented reductions in spasticity, improvements in range of motion, and decreased anxiety in children with cerebral palsy who received regular treatment. For a massage therapist trained in orthopedic assessment, this population offers the chance to apply structural reasoning in a different context: addressing chronic hypertonia, compensatory posture, and restricted movement rather than acute trauma.
Slow, sustained compression along the fiber direction, combined with rhythmic passive movement, can reduce tone more effectively than rapid or forceful techniques. Communication with the child’s broader treatment team is not optional; it is foundational.
Building Trust: The Performance Factor in Pediatric Sessions
Clinical technique accounts for only part of what determines the success of a session. Children test boundaries, asking for more pressure, then less, specifically to see if the therapist will respond. This is a developmental strategy for establishing safety, and building trust may consume entire sessions before meaningful manual therapy begins.
Simple strategies make a significant difference: letting the child choose the starting position, offering a timer so they know how long a technique will last, using age-appropriate language. The performance of the therapy itself is inseparable from the relational context in which it occurs. Parents should be present during sessions, providing emotional security and learning massage techniques they can continue at home.
When that fidgeting child hops down from the treatment table and tells a parent they want to come back next week, something has gone right. A child who trusts the process, a body that is healing well, and a therapist who understood what that particular body needed.
How to Track Your Massage Progress in a Therapeutic Setting
The Shift from Subjective Relief to Clinical Data
I founded RSM International Academy with the belief that massage therapy should be elevated to a precise clinical science. In our massage workshops here in Thailand, we impress upon our students that repairing the human body requires more than intuition. It requires a baseline, a strategy, and a rigorous method of recording changes over time.
Tracking progress is not merely about record-keeping, however, it also requires validation. When we treat a rotator cuff injury or chronic lumbar pain, we need to know if the tissue changes are temporary fluid displacement or genuine structural remodeling. We need to know if the range of motion improvements are neurological adaptations or mechanical releases. Without robust tracking mechanisms, we are essentially guessing.
Structuring Clinical Notes for Measurable Results
The foundation of tracking lies in how we document the encounter. In many spa environments, notes are cursory. For a medical professional, this is insufficient. Detailed charting is the primary tool used to bridge the gap between sessions.
Effective documentation ensures continuity of care. If a patient returns after three weeks, relying on memory is negligence. We must approach documentation with the rigor a surgeon applies to operative reports. Every session is an experiment where we apply a variable (treatment) to a subject and observe the result.
Implementing the SOAP Method in Massage
The SOAP note format remains the gold standard for medical documentation. To track true progress, we must adhere strictly to this structure.
- Subjective: This includes the location of pain and functional limitations. “Pain in shoulder” is vague; “Pain in right anterior deltoid when reaching for a seatbelt” is a trackable metric.
- Objective: This section distinguishes the clinician from the amateur. Here we record palpable findings like tissue texture abnormalities and trigger point locations. Crucially, we must include quantifiable data, such as goniometric measurements.
- Assessment: Based on the SOAP data, is the condition improving or regressing? This is where you correlate objective findings with the patient’s history.
- Plan: This details the future course, specifying frequency, techniques, and self-care homework.
By rigidly adhering to the SOAP format, the note becomes a longitudinal study of the recovery process.
Objective Metrics Beyond the Pain Scale
While the Visual Analog Scale (0-10) is standard, it is often unreliable due to the subjective nature of pain. We cannot rely solely on the patient’s perception to track progress. We must prioritize functional markers.
Range of motion is perhaps the most honest metric. If a client improves from 110 to 125 degrees of shoulder flexion, you have indisputable proof of efficacy. We also evaluate tissue quality. While harder to quantify, describing compliance changes in your notes (e.g., “severe fibrotic limitation” vs. “moderate hypertonicity”) creates a comparative record essential for long-term management.
Leveraging Massage Software and Online Tools
With the multitude of digital options available, selecting a platform can feel overwhelming. Generally, the objective is to find a system that minimizes administrative time while maximizing clinical insight. While we do not endorse specific products, several platforms are frequently discussed by professionals in the field for their specific features:
- Noterro: This platform is often cited by manual therapists for its robust charting capabilities, specifically its body-chart annotations which allow practitioners to draw directly on a diagram.
- MassageBook: This is frequently mentioned as a solution for studios that need to manage multiple staff members, often noted for integrating soap note features with scheduling and marketing tools.
- Cliniko/Jane App: These are popular choices within multidisciplinary clinics. They are often utilized to facilitate integrated care between massage therapists, physiotherapists, and chiropractors.
Ultimately, effective therapy software should do more than just store information; it should present data in a way that supports your clinical decision-making process.
Continuity of Care and Tissue Response
The true power of software tools becomes apparent when treating chronic conditions. Rehabilitation is rarely linear. When a patient presents with a flare-up, digital tools allow you to filter by symptoms or dates, potentially revealing that a specific modality used previously precipitated a similar reaction. This insight allows you to adjust the current treatment plan immediately.
We must constantly evaluate whether the services we provide are generating the desired physiological change. If we apply deep tissue release for three sessions with no change in function, the data tells us to pivot. Massage is an adaptive practice; we look for “micro-wins,” such as increased standing time or reduced headache frequency. These nuances are easily lost if not explicitly recorded.
Elevating Practice: From Intuition to Intelligence
In sports medicine, credibility hinges on results. We elevate the standard of care by combining rigorous manual assessment with efficient massage software and management tools. Whether you use sophisticated online platforms or a meticulous notes system, the discipline of recording and reviewing your approach is what separates the elite therapist from the average practitioner. Tracking progress ensures that our hands are guided by intelligence, not just intuition.
Developing a Massage Treatment Plan: A Clinical Approach
Successful clinical outcomes in sports medicine are rarely the result of intuition alone. They are the result of strategy. During RSM’s Trigger Point Therapy Course, students acquire the ability to formulate a cohesive approach. A single session can provide temporary relief, but sustainable recovery requires a treatment plan.
In my experience working with elite athletes, I have found that patients do not merely seek the alleviation of symptoms; they seek a resolution to the functional limitations causing them. Whether I am treating a footballer with a hamstring strain or an office worker with chronic neck tension, the physiological principles remain constant. We must respect tissue healing times and load management.
A plan is not a rigid script, however, it is a dynamic hypothesis we must test and refine. When a massage therapist moves beyond the “routine” and thinks in terms of long-term tissue adaptation, they elevate their practice from a service to a healthcare intervention.
The Clinical Role of the Massage Therapist
The perception of our field often fluctuates between luxury and necessity. For the clinician, the definition is precise: we manipulate soft tissue to elicit a specific physiological response. This might be maximizing blood flow to an ischemic area or reducing neural tone in a hypertonic muscle.
When a student arrives at our school, they often possess excellent manual skills but lack the structural framework to apply them over time. They know how to treat a shoulder today, but struggle to articulate what that shoulder needs three weeks from now. This is where education regarding proper planning becomes vital.
We must view the massage therapist as a manager of recovery. We are responsible for monitoring the dosage of manual pressure and the frequency of intervention. The body adapts to stimuli specifically imposed upon it. If the stimulus is too infrequent, adaptation does not occur. If it is too aggressive, the tissue fails. The goal is to move clients from a state of pain and dependence to a state of independence.
Creating Effective Treatment Goals
The foundation of any clinical strategy is the assessment. We cannot map a route without starting coordinates. Before creating a plan, we must conduct an evidence-based assessment using orthopedic testing and functional movement screening.
Once we have this data, we can begin creating effective treatment goals. These benchmarks allow us to determine if the therapy is working. A vague goal like “fix the back” is insufficient. A clinical goal is specific: “increase lumbar flexion by 15 degrees and reduce pain scale ratings from 8/10 to 3/10 within four weeks.”
If we reach the four-week mark without improvement, the plan has failed, and we must pivot. This accountability separates clinical massage from recreational bodywork. We generally categorize goals into two phases:
- Short-Term Goals: Focus on symptom management, pain reduction, and restoring initial range of motion. This is the acute phase where inflammation management is paramount.
- Long-Term Goals: Focus on return to function, strength integration, and prevention of recurrence. This often involves collaboration with other professionals to ensure the patient can withstand daily loads.
Designing Comprehensive Treatment Plans
A comprehensive approach recognizes that the body heals in phases. Treatment plans must mirror the stages of tissue healing: acute, proliferative, and maturation.
In the acute phase, the objective is protection. Massage techniques are modified to avoid exacerbating inflammation. We might focus on lymphatic drainage or treating compensatory structures. As we move into the proliferative phase, where new tissue is being generated, the treatment shifts. We become concerned with collagen alignment, introducing friction techniques to ensure new tissue forms functionally.
Finally, in the remodeling phase, the tissue must be stressed to become strong. The therapy here is deeper and combined with active movement. Designing a plan requires understanding this pathology. It informs why we choose myofascial release on day one but eccentric loading on day twenty. It provides the science behind the art.
Establishing a Realistic Treatment Schedule
Compliance is one of the most difficult aspects of clinical practice. You may design the perfect protocol, but if the patient cannot commit, the plan is theoretical. Establishing a realistic treatment schedule requires honest communication.
When determining frequency, we look for the minimum effective dose. For chronic conditions, a single session once a month is rarely sufficient to reverse maladaptive patterning. We often require a “loading phase” – perhaps two sessions a week – to break the pain-spasm cycle.
Once acute symptoms subside, the treatment schedule tapers. We move to once a week, then once every two weeks. This tapering proves to the patient that our goal is their independence. We must also consider the “washout period.” If a patient feels relief for three days but pain returns on the fourth, scheduling appointments seven days apart leaves them in a deficit. In such cases, a twice-weekly schedule is clinically necessary until the window of relief extends.
Integrating a Rehabilitation Plan
A session lasts perhaps sixty minutes. The patient spends the rest of the week treating themselves, positively or negatively. A robust strategy must extend beyond the clinic. This brings us to the importance of the rehabilitation plan or home care protocol.
Education is a powerful analgesic. When a patient understands their injury, anxiety decreases, which often correlates with lower pain perception. We integrate homework to bridge the gap between sessions. This might include simple mobility exercises or self-release techniques.
For the student building a career, mastering this advice is as important as hands-on skills. If a client leaves without knowing what to avoid or how to help themselves, the therapist has done only half the job.
When to Modify Treatments
Rigidity is the enemy of recovery. The human body is complex. There will be times when a patient arrives with a flare-up, or conversely, has healed faster than anticipated. We must be willing to modify treatments.
Re-assessment is continuous. At the start of every session, we check benchmarks. Has the range of motion improved? Is the pain reduced? If the answer is no, we analyze why. If a specific modality within the massage therapy treatment is not yielding results, we change it. We might switch from trigger point therapy to instrument-assisted mobilization. The plan guides us, but the patient’s response dictates the daily tactics.
The Professional Evolution
For those dedicated to this field, planning care transforms the work. You are no longer just rubbing backs; you are engaging with the physical reality of anatomy. At RSM, we emphasize that the ability to construct these plans builds a thriving practice. Patients return because they see a progression.
This clinical structure allows us to interface respectfully with other medical professionals. When you can send a progress report to a doctor outlining your assessment and therapy treatment outcomes, you validate the profession. Massage therapy becomes a viable, evidence-based component of healthcare.
To ensure clinical efficacy, every plan should contain these essential elements:
- Subjective & Objective Assessment: The patient’s narrative combined with measurable physical data.
- Goal Setting: Establishing both short-term and long-term benchmarks.
- Intervention Strategy: Selection of specific massage modalities and the rationale for their use.
- Frequency & Duration: The proposed treatment schedule based on physiological healing.
- Re-evaluation Protocols: Check-in points to measure progress and modify the approach.
- Home Care: Educational support to facilitate self-management.
By adhering to this structure, we ensure that every hour spent with a patient contributes meaningfully to their health. We move away from guesswork and toward a standard of excellence.