RSM Blog: Manual Therapy Techniques
Debunking Common Myths About Deep Tissue Massage
I sometimes encounter students in our Deep Tissue Massage Course who believe that an effective massage must be an ordeal of physical endurance. This perspective is often reinforced by a misunderstanding of how the nervous system and musculoskeletal structures interact during manual work. Many aspiring practitioners believe that for a session to produce results, it must involve significant discomfort. However, this belief ignores the physiological reality of muscle guarding. Various myths regarding tissue manipulation persist; yet, force is a poor substitute for accuracy.
The Deep Tissue Massage Pain Fallacy
The most pervasive misconception suggests that the effectiveness of a deep tissue massage is directly proportional to the amount of intensity a client experiences. This logic is fundamentally flawed from a neurological standpoint. When a practitioner applies pressure that exceeds the threshold of the individual, the body perceives this as a threat. Specifically, the sympathetic nervous system triggers a protective response. This causes the muscles to contract reflexively to shield the underlying structures. Consequently, the practitioner is no longer working on pliable tissue but is instead fighting against the body’s own defensive mechanisms.
In my clinical experience, the most successful outcomes occur when the pressure remains just below the threshold of protective guarding. We teach students to monitor the client’s breath and subtle muscle twitches. If the client is holding their breath or tensing their jaw, the pressure is too high. This leads to a paradoxical effect where the massage therapy creates more tension than it resolves. By staying within a therapeutic window, the student can access deeper layers of fascia and muscle without triggering a systemic stress response.
Massage Myths Regarding Metabolic Toxins
Another persistent myth involves the idea that manual tissue work flushes out lactic acid or unspecified toxins from the body. From a biochemical perspective, lactic acid is a metabolic byproduct that the system clears naturally. Research in modern exercise physiology shows that lactate is also used as a primary fuel source by the heart, brain, and non-working muscles. Mechanical pressure on muscle tissue does not significantly accelerate this metabolic clearance. Instead, the perceived benefits of a session often stem from improved local blood circulation and the modulation of signaling in the central nervous system.
The toxin narrative is often used as a marketing tool in a spa environment; however, it lacks a basis in sports medicine. When we perform deep tissue applications, we are primarily influencing the mechanical properties of the fascia and the tonus of the muscular system. This process involves slow-adapting mechanoreceptors, such as Ruffini endings and Merkel discs, which respond to steady compression and lateral stretch. This is a neuro-mechanical shift, not a chemical purification.
Common Misconceptions in Manual Therapy:
- Bruising is a sign that the tissue massage successfully reached the deep tissue layers.
- Drinking water after a session is necessary to wash away released poisons.
- Deep tissue work is only appropriate for people with high pain tolerances.
- A therapist should always focus exclusively on the point of discomfort.
Applying Tissue Massage For Clinical Therapy
The goal of a technical tissue massage is to restore functional movement by addressing the kinetic chain. If a student uses an aggressive massage style to “crush” muscle tension, they often cause micro-trauma to the superficial capillaries and nerves. This leads to bruising and localized inflammation. At RSM International Academy, we focus on specific, layer-by-layer palpation to address the root cause of the problem.
We use deep tissue work as a tool to explore interconnected webs of fascia. Addressing therapy myths is essential for providing high-quality care. By using slow, sinking pressure, we can reach the deep stabilizers without causing the superficial layers to seize up. This approach produces lasting relief from chronic pain because it addresses the mechanical source of the dysfunction rather than just the symptoms. Once we move past the massage myths, we can focus on the real work of clinical therapy.
Adapting Massage for Different Body Types
The Limitations of Standardized Massage
A fundamental error in how massage is taught globally is the reliance on a set sequence. This approach assumes human anatomy is a constant variable. In practice, this is false. The variation in skeletal structure, muscle density, and tissue consistency among individuals is immense. When a massage therapist applies a standardized routine to variable anatomy, the results are often mediocre.
In RSM International Academy's massage workshops in Thailand, we teach that effective therapy requires constant adaptation. The force vectors required to release a hypertonic rhomboid in a dense athlete are useless on a fragile ectomorph. Conversely, sharp elbow pressure on deep spinal erectors will cause guarding if applied to a client with a lower pain threshold. Success in this field relies on reading the structure before applying the technique.
The Ectomorph Body: Precision Over Power
The ectomorph somatotype presents specific challenges. These individuals typically possess a delicate skeletal frame and lower muscle mass. Consequently, their bony landmarks are prominent and structurally exposed.
When working with an ectomorph body, the margin for error is slim. The distance between the skin surface and the periosteum is minimal. Heavy compression here does not release tension; it compresses the bone against the table. This triggers a sympathetic nervous system response, causing the client to flinch.
For these clients, I emphasize specificity over general force. Instead of broad, heavy strokes, we must use precise, focal pressure. We target the muscle belly without grinding over the skeletal prominence. Furthermore, ectomorphs often lack insulating adipose tissue, making their superficial fascia more accessible. We must adjust our engagement speed, entering the tissue slowly to allow the nervous system to accommodate the touch.
Mesomorphs: Strategies for Dense Tissue Massage
In contrast, the mesomorph presents a robust musculoskeletal system. These clients are naturally muscular, creating significant density within the myofascial layers. Treating this body type requires a shift in mechanics. A simple effleurage will simply slide over the surface, failing to address underlying muscle tension.
To effect change here, we utilize dense tissue massage strategies. The primary challenge is not just thickness but tone. If a therapist tries to force their way through with brute strength, the client’s muscle will fight back. Instead, we use a “sink and wait” approach. We apply heavy load perpendicular to the fiber direction and wait for the autonomic nervous system to lower the tonus.
This is critical for deep tissue work. For athletes with tissues adapted to high-velocity impact, we often employ sports massage techniques that utilize active movement. By having the client actively lengthen the muscle while we apply stripping pressure, we use their internal mechanics to generate necessary shear force.
Endomorphs: Palpation and Sculpting Massage
The endomorph somatotype is characterized by a higher percentage of adipose tissue and a wider skeletal structure. Clinically, this presents a palpation challenge. The subcutaneous fat buffers the tactile feedback that tells a massage therapist where the tension lies.
Many inexperienced therapists use too little pressure on endomorphs, assuming the tissue is soft. However, adipose tissue is not highly innervated with pain receptors. This allows for, and requires, firmer pressure to transmit force down to the muscle belly.
This is where the concept of sculpting massage becomes relevant in a therapeutic context. It is not about body contouring for aesthetics; it is about defining the boundaries of muscle groups that are not visually apparent. We must displace the adipose layer laterally to fixate the muscle underneath. Without this displacement, the massage force disperses into the soft tissue, providing no mechanical benefit to the contractile fibers.
Adjusting Therapy for Structural Asymmetry
Adapting to a body unique to the individual is not just about weight; it is about skeletal geometry. Structural variances dictate where mechanical stress accumulates.
Consider a client with structural kyphosis (rounded upper back). The thoracic spine is fixed in flexion, and the rhomboids are locked in a “long-weak” position. Standard massage techniques often involve digging into the upper back pain. However, aggressively stripping these over-stretched muscles can destabilize the area. The tissue here needs facilitation, not inhibition.
Conversely, in clients with lumbar lordosis (swayback), the pelvis tilts anteriorly. A generic lower back massage that focuses solely on the lumbar erectors often fails. The erectors are tight because they are compensating for the pelvic tilt. To resolve this, we must address the anterior hip. Releasing the psoas allows the pelvis to neutralize, naturally reducing lower back tension. This represents the difference between a relaxation rub and clinical massage therapy.
Clinical Protocol: Matching Technique to Tissue
To systematically adapt our treatments, we categorize our approach based on tissue interaction.
- The Anchor and Stretch:
For clients with high elasticity, simple gliding strokes slide over the problem. We use “anchoring,” pinning the distal end of a muscle and pushing the belly proximally. This creates a shear that forces layers to separate, vital for effective tissue massage. - The Stack and Sink:
For dense deep tissue (Mesomorphs), we stack our joints: shoulder over elbow. This skeletal alignment allows us to deliver significant force without muscular effort. We sink using body weight, protecting the therapist while delivering necessary depth. - The Scoop and Lift:
For clients with adherence between skin and muscle (often in dehydrated types), we use lifting techniques. Instead of compressing, we lift the muscle away from the bone to rehydrate fascial layers.
The Precision of Personalized Care
The idea that “massage is massage” hinders our industry. A personalized massage is a clinical necessity. The efficacy of our work depends on how well we match our mechanics to the client’s anatomy.
By respecting the fragility of the ectomorph, engaging the density of the mesomorph, and navigating the layers of the endomorph, we elevate our practice. At RSM International Academy, we teach students to analyze the body, assess the tissue, and adapt their art. This tailored approach is precise, logical, and ultimately, far more effective.
Understanding the History of Shiatsu Massage Practice
At RSM we approach manual therapy with a rigorous focus on anatomy and physiological outcomes. While our curriculum prioritizes sports medicine and functional correction, understanding the lineage of our tools is essential for any elite practitioner. The manual techniques utilized today did not appear in a vacuum; they are the result of clinical trial, observation, and the synthesis of Eastern empirical experience with Western anatomical science.
The origins of shiatsu massage offer a fascinating case study in this convergence. It is not merely a story of ancient tradition but a technical evolution where practitioners adapted their methods to align with a changing understanding of the human body. By examining this history, students in our Shiatsu Massage Course gain insight into why specific pressure techniques effectively modulate neuromuscular tone and how the integration of varying styles of medicine creates a more robust clinical framework.
Tracing the History of Shiatsu and Traditional Roots
The foundations of shiatsu lie deep within the exchange of medical knowledge between China and Japan. During the Nara period, Buddhist monks introduced traditional Chinese Medicine (TCM) to Japan, bringing with them herbal medicine, acupuncture, and a form of manual manipulation known as Tui Na. In Japan, Tui Na evolved into Anma. For centuries, Anma was the dominant form of manual therapy, focusing on the flow of Ki (energy) through meridians.
However, a distinct shift occurred during the Edo period. The government mandated that Anma be performed largely by the blind as a social welfare measure. While this preserved the profession, it eventually altered the public perception of the practice. By the Meiji Restoration, Anma became associated more with relaxation than clinical medicine. This shift necessitated a reaction from therapists who viewed manual manipulation as a serious therapeutic intervention. Consequently, a new group of therapists began to distance themselves from the term “Anma,” seeking to re-establish the clinical credibility of their work through a more structured approach.
Therapists sought a method that relied less on the rubbing and friction characteristic of Anma and more on sustained, perpendicular pressure. The term “shiatsu“, meaning “finger pressure”, emerged to describe this technique. The practices of shiatsu distinguished themselves by utilizing body weight rather than muscular force. By stacking the joints and using gravity, the therapist could deliver deep, stable pressure into the tissues. This mechanism stimulates the parasympathetic nervous system, reducing muscle hypertonicity and lowering cortisol levels.
Tokujiro Namikoshi and the Formalization of Shiatsu Therapy
The formal recognition of shiatsu as a distinct legal and medical entity is largely credited to Tokujiro Namikoshi. His contribution was not just in technique but in systematization. Namikoshi faced the challenge of defining shiatsu therapy in a way that satisfied the rigorous demands of the Japanese Ministry of Health and Welfare.
Namikoshi established the Japan Shiatsu College in 1940, adopting a decidedly Western anatomical focus. He moved away from the meridian theory that underpinned Anma and acupuncture. Instead, he proposed a system based on “reflexes.” He argued that by applying pressure to specific points, a practitioner could elicit a visceral-cutaneous reflex, influencing internal organ function through the nervous system.
This logic mirrors the somato-visceral reflex arcs we study in modern physiology. Namikoshi’s emphasis on the nervous system allowed shiatsu to be legally defined as a distinct practice, separate from Anma and Western massage. In 1955, the Ministry of Health and Welfare officially recognized shiatsu. Namikoshi famously stated, “The heart of shiatsu is like a mother’s love,” yet his technical legacy is one of rigorous standardization. He mapped out the body using anatomical landmarks, creating a reproducible system for courses and training. This anatomical precision legitimized the profession and paved the way for international expansion.
Shizuto Masanaga and the Rise of Zen Shiatsu
While Namikoshi focused on anatomical structure, Shizuto Masanaga sought to reintegrate the psychological and energetic aspects of the therapy. A professor of psychology, Masanaga believed that the purely anatomical approach missed a critical component of the patient’s experience. He argued that physical tension was often a manifestation of emotional or psychological imbalance.
This divergence led to the development of Zen Shiatsu. Masanaga expanded the meridian system used in acupuncture, proposing that energy channels existed throughout the entire body. He introduced the concept of “Kyo” (deficiency) and “Jitsu” (excess) and taught practitioners to assess the energetic state of the abdomen.
The technical difference in Masanaga’s style is significant. He emphasized “stationary perpendicular pressure” coupled with a two-hand technique: one hand acting as the “mother hand” (stabilizing) and the other as the “child hand” (active). This creates a closed circuit of bio-feedback. From a sports medicine perspective, this two-hand contact enhances proprioceptive feedback, allowing the therapist to sense subtle changes in tissue tone that might be missed with single-point pressure. Masanaga’s philosophy formalized the dynamic interaction between therapist and patient, influencing how many modern shiatsu practitioners approach treatment.
Clinical Perspectives on Massage and Modern Shiatsu
In the 1970s and 80s, expanding interest in alternative and holistic health in the West created fertile ground for Japanese manual therapies. However, this global expansion often led to a fragmentation of techniques. In many Western contexts, shiatsu is marketed broadly as a relaxation massage, stripping away the diagnostic rigor intended by its founders.
Despite this, the core principles remain valid when applied correctly. Research into massage and pressure therapies consistently shows that mechanical deformation of fibroblasts leads to changes in tissue hydration and stiffness. Whether one calls this “releasing blockages” or “reducing fascial densification,” the physiological result of sustained pressure is objectively measurable. The success of shiatsu stems from its ability to mechanically disrupt these densifications while downregulating the sympathetic nervous system.
In my clinical experience, a primary lesson of shiatsu theory is the importance of biomechanical efficiency. The founders realized that using muscular force was unsustainable. They developed a method of delivering force that protected the therapist’s joints while delivering deep pressure. At RSM, we teach a similar efficiency. We utilize gravity and leverage to treat elite athletes. While we may not adhere to specific meridian maps, the fundamental mechanic – stable, perpendicular pressure – is a shared heritage that effectively addresses ischemia and metabolic waste.
The history of shiatsu massage showcases the adaptability of Japanese medicine. It demonstrates a transition from empirical traditions to systematized, anatomically grounded therapy. For students, these are lessons in professional development. A practitioner must be willing to refine their techniques and integrate new evidence to provide the best care. Whether through sports medicine or traditional modalities, the goal remains the same: restoring function and alleviating pain through skilled touch.
Key Historical Distinctions:
- Anma: Precursor to shiatsu, focused on kneading/friction, influenced by TCM.
- Namikoshi Style: Focuses on anatomical reflexes, Western physiology, and distinct legal status.
- Masanaga Style: Reintroduced meridians, psychological diagnostics, and the “mother/child hand” technique.
Developing Treatment Plans in Orthopedic Massage
Many practitioners believe that mastering specific strokes is the key to resolving musculoskeletal issues. However, a technique without a strategy is simply a physical action lacking direction. To truly resolve complex pain patterns, we must shift our focus from isolated techniques to comprehensive strategy, and from addressing symptoms to reverse-engineering the dysfunction. This requires a deep understanding of anatomy, biomechanics, and pathology. When I treat a client, I am not merely looking for tight muscles. I am looking for the “why.” This line of questioning is the bedrock of how I teach students to develop treatment plans in our Orthopedic Massage Course.
Foundations of Clinical Reasoning in Orthopedic Massage
Success depends heavily on clinical reasoning. This cognitive process allows a therapist to filter the vast amount of data a client presents into a coherent course of action. It is insufficient to know where the pain is located. We must understand the mechanism that placed it there.
For instance, when a client presents with lateral knee pain, a novice might immediately treat the iliotibial band. Clinical reasoning dictates we look elsewhere. The iliotibial band responds to tension in the tensor fasciae latae (TFL). If the pelvis is anteriorly tilted, the TFL shortens mechanically, pulling on the IT band. Rubbing the knee provides temporary relief. Correcting the pelvic tilt resolves the issue.
This logic applies to all musculoskeletal conditions. The body operates as a tensegrity structure; a failure in one area forces compensation in another. Clinical success comes from identifying the primary driver rather than chasing symptoms. At RSM, we emphasize that orthopedic massage is defined by the specificity of the assessment, not the depth of pressure.
The process of decision making is linear. We observe gait and posture to gather initial data. This informs the physical assessment, which subsequently informs the strategy. Skipping steps leads to missed information and failed outcomes.
The Role of Patient History in the Treatment Plan
Before we touch the body, we must gather intelligence. The patient history is often more valuable than palpation. It reveals the timeline of the dysfunction. A pain that appeared yesterday requires a different approach than a dull ache that has persisted for a decade.
I ask specific questions to determine the nature of the tissue damage. Is the pain sharp and shooting? This suggests nerve involvement. Is it throbbing? This indicates vascular involvement or inflammation. The answers dictate the safety of the treatment plan. For example, treating an acute ligament sprain with deep friction disrupts the fibrin clot, whereas chronic tendinosis requires friction to restart inflammation. The history tells us where the tissue is in the healing cycle.
We must also define clear treatment goals. These goals must be shared between the practitioner and the client. If expectations do not align with physiological reality, we must educate the client.
Identifying the source of client pain involves differentiating between the site of symptoms and the source of dysfunction. In many cases of lumbar pain, the lower back is merely the victim of a hip dysfunction. If the hip does not extend, the lumbar spine hyperextends. The patient feels pain in the back, but the problem lies in the hip.
Selecting Techniques for Specific Orthopedic Conditions
Once the hypothesis is formed, we select the tools. In orthopedic massage, we have a wide array of techniques. The skill lies in matching the technique to the tissue state.
For adhesive capsulitis, the goal is to increase range of motion without triggering inflammation. Aggressive stretching causes the capsule to thicken protectively. Instead, we use gentle mobilization to free the scapula. Conversely, for lateral epicondylitis, deep transverse friction is appropriate to restart the inflammatory cycle in the degraded tendon. The protocol changes based on the pathology.
Soft tissues respond specifically to mechanical load. Sustained pressure melts fascia, while rhythmic compression reduces tone. We must also consider the nervous system. Pain is an output of the brain. If a client is in a state of sympathetic arousal, their muscle tone remains high. In these instances, the therapy must first down-regulate the nervous system using breathwork or rocking. This nuance is the essence of clinical decision-making.
Addressing injuries requires a phase-dependent approach:
- Acute Phase: Protection and lymphatic drainage.
- Sub-Acute Phase: Controlled mobilization to align collagen.
- Chronic Phase: Strengthening and eccentric loading.
Structuring Therapy and Therapeutic Exercises
Passive treatment is rarely enough to correct lifetime movement patterns. To ensure long-term results, we must integrate active strategies. Therapeutic exercises bridge the gap between manual therapy and functional movement.
When we release a tight muscle, the nervous system gains a new range of motion. However, if the client does not use this range, the brain reverts to the old pattern. We must cement the change through immediate movement. If I release the iliopsoas, I immediately have the client perform a glute bridge. This tells the brain to control the new range.
This integration transforms a simple appointment into a comprehensive rehabilitation plan. We are optimizing the system, not just fixing parts.
Flexibility is often misunderstood. Static stretching can be detrimental if a muscle is tight because it is protecting an unstable joint. In such cases, the treatment plan should focus on stability. For example, in Upper Cross Syndrome, stretching the tight upper trapezius often fails because the deep neck flexors are weak. Strengthening the weak muscles allows the tight muscles to relax permanently.
From Assessment to Massage Application
The transition from assessment to massage therapy must be seamless. The client should feel that every stroke has a purpose.
We structure the session logically. We begin superficially to acclimate the nervous system, then move to specific work on the primary restrictions. Finally, we integrate the work with broader strokes. The therapist must constantly monitor the tissue response. Is the muscle pushing back? Is it melting? This feedback loop allows for real-time adjustment.
Reasoning continues throughout the session. We are constantly testing and re-testing. After releasing the quadratus lumborum, we check spinal flexion. If it has not improved, we re-evaluate. This dynamic approach defines the RSM method.
Orthopedic conditions are rarely linear, and rehabilitation requires patience. We teach clients how to modify daily activities and manage their condition. When a client understands the mechanism of their injury, they become active participants in their recovery. By prioritizing assessment and developing bespoke strategies, we elevate the standard of care from generic routines to true clinical excellence.
Deep Tissue Massage Techniques Explained: A Clinical Perspective
At RSM we approach bodywork with a foundation rooted firmly in sports medicine. Many clients arrive with misconceptions about effective manual therapy, often equating efficacy with the intensity of pain endured. However, true clinical results rely on precision, not just force. In this article, I will have deep tissue massage techniques explained as a systematic method for restoring structural integrity and physiological function.
I frequently observe that chronic pain patterns are rarely isolated. A complaint of shoulder tension often traces back to pelvic instability. The body operates as a tensegrity structure; a restriction in one area alters the tension balance system-wide. Consequently, treating the site of pain without addressing the underlying fascial restrictions yields only temporary results. Our Deep Tissue Massage Course shifts the focus from general relaxation to specific functional correction.
Deep Tissue Massage Techniques Explained Through Anatomy
To understand these methods, we must visualize the body’s layers. The term “deep tissue“ is often misused to describe heavy pressure. In reality, it refers to targeting the sub-layers of muscle and fascia that support posture.
Beneath the superficial fascia lies the deep fascia, a dense layer compartmentalizing muscle groups. This is where many chronic restrictions reside. When deep tissue massage techniques explained correctly are applied, the therapists do not push through the body; they sink to the appropriate depth. Attempting to force access to deep muscles without warming superficial layers triggers a protective reflex called “muscle guarding.” Consequently, the therapist ends up fighting the body rather than working with it.
Effective therapy requires hooking the tissue. Once the correct depth is achieved, the stroke involves a shearing force. This separation is vital for breaking down adhesions. When individual muscle fibers glide freely, the muscle contracts efficiently. When glued together by scar tissue, performance drops. By applying a slow, oblique angle of pressure, we engage the collagen fibers, stimulating the ground substance to become more fluid. This reduces friction and restores the natural slide-and-glide mechanism essential for pain relief.
Integrating Myofascial Release into Massage Treatments
While often categorized separately, myofascial release is intrinsic to effective deep work. Fascia is a continuous web surrounding every structure. Trauma or poor posture tightens this web, exerting immense pressure on sensitive areas.
Myofascial restrictions do not show up on X-rays, yet they are a primary source of undiagnosed pain. A standard massage stroke might glide over these restrictions. Conversely, myofascial techniques engage the barrier of resistance and wait. We apply sustained tension until the piezoelectric effect softens the collagen matrix. This is critical for conditions like IT band syndrome, where the issue is the densification of connective tissue rather than simple muscle tension.
Targeted Trigger Point Therapy
Chronic pain patients require a strategy to interrupt the pain-spasm-pain cycle. When a muscle is chronically contracted, blood flow is restricted (ischemia), causing metabolic waste buildup that irritates nerve endings. To break this cycle, we employ specific strategies.
A trigger point is a hyperirritable spot within a taut band of skeletal muscle. When compressed, it produces a “twitch response” and refers pain elsewhere. Treating these points requires Ischemic Compression: applying direct pressure to temporarily cut off blood supply. Releasing this pressure prompts the body to flood the area with fresh, oxygenated blood, washing away pain-causing metabolites.
However, treating nerve pain (neuralgia) requires a different approach. Nerves are sensitive to compression. Therefore, we use specific point therapy to address the interface between the nerve and surrounding soft tissue. For example, in Cluneal Neuralgia, we release the thoracolumbar fascia to free the nerve from entrapment. This creates space and reduces irritation without applying direct, aggravating pressure to the nerve itself.
Friction and Stretching Techniques in Massage
When dealing with chronic tendinopathies or dense fibrosis, gliding strokes are insufficient. We must employ friction techniques. Cross-fiber friction applies pressure perpendicular to the tissue fibers. This induces a localized inflammatory response to restart healing and physically realigns haphazard collagen fibers, restoring tensile strength to tendons.
Passive treatment has limitations. To create lasting changes, the client must be an active participant. At our clinic, we integrate active engagement and stretching techniques directly into the session.
Techniques like Pin and Stretch involve the therapist manually pinning a shortened muscle while the client moves through a range of motion. This active movement strips away fibrosis more effectively than passive pressure. Similarly, Muscle Energy Techniques (MET) utilize the body’s own neurological reflexes to relax tight muscles, allowing us to gain mobility without brute force.
Elevating the Standard of Massage
Deep tissue massage is a sophisticated modality bridging relaxation and medical rehabilitation. It is not about how hard one pushes, but how effectively one communicates with the physiological systems. By understanding the layers of the body and the mechanics of the nervous system, we provide profound relief.
At RSM International Academy, whether dealing with an elite athlete or a standard spa client, the principles remain the same: assess accurately and treat specifically. Through the precise application of these techniques, we do not just alleviate symptoms; we facilitate the body’s innate ability to heal.
How to Identify Muscle Knots in Practice
The Physiological Basis of Muscle Knots
In sports medicine, what patients colloquially call a “knot” is scientifically defined as a myofascial trigger point. While it feels like a hard lump, it is actually a distinct physiological crisis occurring within the muscle fibers. Understanding this mechanism is the prerequisite for effective treatment.
A trigger point begins at the microscopic level of the sarcomere. Under stress or trauma, the sarcoplasmic reticulum malfunctions and releases excessive calcium. This flood of calcium causes the sarcomeres to sustain a continuous contraction. This contraction compresses local capillaries, cutting off oxygen supply to the tissue.
As a result, the area suffers from ischemia. Without oxygen, the cells cannot produce the ATP necessary to pump the calcium back out and relax the fiber. A metabolic cycle ensues: the muscle stays contracted because it lacks energy, and it lacks energy because the contraction restricts blood flow. This ischemic feedback loop creates the palpable nodule we recognize as a muscle knot. At RSM International Academy, our Trigger Point Therapy Course teaches that that effective therapy acts to break this chemical cycle, restoring circulation to the starved tissue.
How to Identify Muscle Knots
Learning how to identify muscle knots requires more than just finding a sore spot. A true trigger point has specific characteristics that distinguish it from general muscle tightness or spasms. I teach a specific palpation sequence to ensure accuracy.
The primary indicator is the “taut band.” When you palpate across the fiber direction, you will feel a ropy, hardened texture distinct from the surrounding healthy tissue. The knot itself is the most tender point located along this band. When pressure is applied, two distinct reactions confirm the diagnosis:
- The Jump Sign: The patient involuntarily flinches due to the sharpness of the pain.
- The Local Twitch Response: A transient, visible spasm of the muscle fibers. This reflex confirms the sarcomeres are in a hyper-irritable state.
Palpation Techniques
To accurately identify muscle dysfunction, we use different techniques depending on the anatomy:
- Flat Palpation: Used for muscles pressed against bone, like the paraspinals. You slide fingertips across the fibers to feel for a “snap” or change in density.
- Pincer Palpation: Essential for muscles that can be lifted, such as the upper trapezius or sternocleidomastoid. You grasp the belly of the muscle to locate the indurated nodule.
Differentiating Knots from Other Structures
Novice therapists often misidentify lymph nodes or lipomas as muscle knots. This mistake can lead to ineffective massage or potential injury.
Lymph nodes, common in the neck and axilla, feel like small, movable beans. Unlike a muscle knot, they do not produce a twitch response or referred pain. Lipomas are fatty deposits that sit between the skin and fascia; they are generally doughy and painless. A trigger point, conversely, has a hard, unyielding “end feel” and is embedded deep within the muscle. If a lump feels attached to the bone or pulses, do not treat it. Refer the client to a specialist.
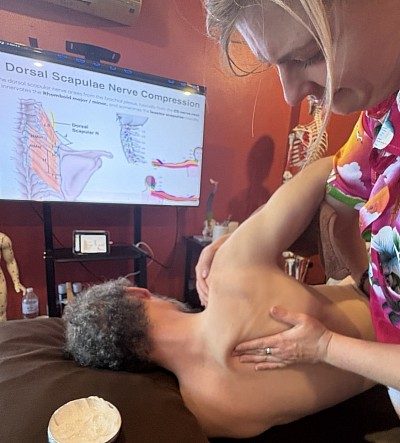
Common Locations: Upper Back and Shoulder
In modern clinical practice, the upper back and neck are the most frequent sites for dysfunction. The anterior head carriage common in office workers forces the posterior chain to maintain an isometric contraction to support the skull. This chronic load creates a fertile environment for tension.
The upper trapezius is the usual suspect for shoulder knots. However, the Levator Scapulae, which is situated deep to the trapezius, is often the true culprit for stiffness. Because it elevates the scapula, it becomes fibrotic when shoulders are chronically hiked due to stress.
Furthermore, pain in the Rhomboids (between the shoulder blades) is frequently secondary to tight chest muscles. The Pectoralis Major pulls the shoulders forward, locking the Rhomboids in a stretched position. Consequently, the knots found in the back are often a reaction to tension in the front. To effectively identify the source, one must assess the entire upper torso.
Advanced Assessment: Referred Pain Patterns
To successfully treat back pain or headaches, we must understand that pain is often a liar. The location of the symptom is rarely the source. Active trigger points produce “referred pain” – discomfort felt at a distance from the knot.
For example, a trigger point in the upper trapezius often sends a referral pattern up the neck into the temple. A client may seek relief for a headache, but the cause lies in the shoulder. Similarly, points in the infraspinatus can refer deep ache into the front of the shoulder, mimicking tendonitis.
We also distinguish between active and latent points. Active points cause spontaneous pain. Latent points are only painful when pressed but restrict movement and weaken the muscle. Treating only the active points provides temporary pain relief, but ignoring latent points invites recurrence.
Treatment and Release Techniques
At RSM International Academy, our philosophy integrates Western anatomy with precise manual techniques. We do not believe in “forcing” a knot to release. Aggressive pressure triggers the sympathetic nervous system, causing the muscle to guard and tighten further.
Instead, effective release requires “melting” the restriction. We apply pressure to the barrier of resistance and wait for the tissue to yield. As the ischemia resolves and blood flow returns, the sarcomeres disengage. This approach works with the nervous system, not against it.
Knowing the direction of the muscle fibers is critical. You must palpate across the fibers to find the taut band, but often strip parallel to the fibers to flush metabolic waste.
The Path to Resolving Trigger Points
The ability to identify muscle knots elevates a therapist from a general practitioner to a specialist. It requires a synthesis of anatomical knowledge and tactile sensitivity. By tracing the taut band, eliciting the twitch response, and mapping referred pain, we address the root cause of the dysfunction. Whether treating the upper back, neck, or lower limbs, the goal remains the same: restore oxygen, restore length, and restore function. This causal approach ensures lasting recovery rather than fleeting relief.
Frequently Asked Shiatsu Massage Questions: A Clinical Perspective
At RSM International Academy, I often encounter a fundamental misunderstanding regarding Japanese manual therapy. Many view it simply as relaxation. But, from a sports medicine perspective, what is shiatsu? It is a rigorous, anatomical method designed to restore homeostasis. It bridges the physiological principles of Western medicine with the energetic framework of Traditional Chinese Medicine (TCM).
The body functions not as isolated parts but as an integrated unit. When a patient reports pain, a novice therapist might treat the symptom. An expert looks for the cause. This distinction drives our our Shiatsu Massage Course. We teach that structural alignment dictates the flow of energy and fluid. Consequently, the shiatsu therapy we practice is specific, calculated, and deeply clinical.
Understanding Shiatsu Diagnosis and Root Causes
A core component of our methodology is shiatsu diagnosis. Unlike Western pathology, which labels a disease, this diagnostic approach assesses the balance of the body. We look for “Jitsu” (excess tension) and “Kyo” (weakness).
For instance, a tight lower back often compensates for inactive glutes. Treating only the tight area offers fleeting relief. However, addressing the weak link restores pelvic stability. This causal logic is vital. We observe how postural distortions inhibit the meridians, blocking the body’s natural recovery mechanisms. Therefore, the goal is not merely to press hard, but to press accurately to correct these imbalances.
The Mechanics of a Shiatsu Treatment
Clients often ask how a shiatsu treatment differs from standard oil therapies. The primary distinction is the application of perpendicular pressure without lotions. The client remains fully clothed, allowing for dynamic joint mobilizations that would be slippery or difficult with oil.
The technique relies on finger pressure. We do not rub the skin. Instead, we sink vertically into specific acupressure points (tsubo). This static compression stimulates deep mechanoreceptors. As a result, the parasympathetic nervous system engages, lowering muscle tonus and heart rate.
We teach that effective shiatsu requires “melting” into the tissue. If the pressure is too sharp, the body guards against it. Conversely, correct depth creates a “good pain” – a sensation of release where the body acknowledges the correction.
Is Shiatsu Massage Distinct from Western Modalities?
While the term shiatsu massage is frequently used, professionally, we distinguish it from Western massage. Western styles typically utilize strokes like effleurage to increase blood flow parallel to muscle fibers.
In contrast, shiatsu employs static pressure and cross-fiber manipulation. This aligns more closely with myofascial release. The benefits extend beyond the musculoskeletal system. By targeting points along the meridians, we influence autonomic regulation. This makes it highly effective for stress-related health conditions, including insomnia and digestive issues. The compression acts as a pump, flushing venous blood and accelerating tissue repair.
Protocols for Treatment and Frequently Asked Safety Questions
Determining the number of treatments needed depends on tissue physiology. Frequently asked questions often concern frequency. For acute strains, frequent sessions prevent scar adhesion. However, for chronic issues like frozen shoulder, a single session is insufficient. The fascial patterns took years to form; they require consistent input to resolve.
Safety is also a priority. Generally, this is a safe modality. However, we do not apply deep pressure over varicose veins or open wounds. Pregnancy requires specific caution; a qualified specialist knows which points to avoid to prevent inducing labor.
Ultimately, the outcome depends on the shiatsu therapist. At RSM, we emphasize that the therapist must cultivate focused presence (“Mushin”). We train students to use body weight rather than arm strength. This ensures the pressure is stable and deep, inviting the client’s muscles to release rather than resist.
Whether you are a prospective student or a client, understanding these technical nuances is essential. Shiatsu is not magic; it is a sophisticated interaction between anatomy and physiology. We invite you to experience this profound modality, where every question leads to a better understanding of clinical recovery.
Understanding the Difference Between Massage and Myofascial Release
Defining the Mechanics of Deep Tissue Massage
Effective manual therapy requires understanding the layers of the human body. Students often confuse modalities, yet the physiological targets are distinct. When we address the belly of the muscle directly, we are operating within the realm of massage.
Deep tissue massage focuses on the contractile element: the sarcomere. Overworked muscles accumulate metabolic waste, leading to local ischemia and hypertonic “knots.” The primary goal of this therapy is to restore circulation to these fibers.
We achieve this through rhythmic mechanical pressure. By applying strokes that follow the muscle fibers, we physically pump venous blood out of the tissue. Fresh, oxygenated blood rushes in to replace it, flushing waste and separating stuck fibers. Consequently, the muscle relaxes. The application involves lubrication in the form of oils or waxes to allow the hands to glide. This fluid movement is essential for the circulatory effect that characterizes traditional sports and remedial massage.
The Science Behind Myofascial Release
In contrast, myofascial release targets the fascial system. Fascia is the connective tissue matrix surrounding every muscle, bone, and organ. Healthy fascia is hydrated, allowing muscles to slide. However, trauma or poor posture causes the ground substance of the fascia to dehydrate and thicken, gluing muscle layers together.
Standard massage techniques often fail here. Because massage uses lubrication, it slides over these restrictions. Myofascial release work requires no lubrication. The therapist must achieve a “lock” on the skin to engage the underlying connective tissue. We do not slide; we drag.
This sustained shear force exploits thixotropy. When we introduce heat and pressure to the dense fascia, it transforms from a gel to a sol (liquid) state. This allows the collagen fibers to elongate. If the therapist releases tension too quickly, this piezoelectric effect does not occur, and the restriction remains.
Contrasting Fluidity with Structural Drag
The difference between massage and myofascial release is ultimately a matter of time, friction, and intent. Confusing these two modalities leads to sub-optimal results.
During a massage, the rhythm is faster, stimulating the nervous system and forcing fluids through the body. The sensation is often “good pain” and immediate relief. Conversely, an MFR treatment is slow. A single release may take five minutes. The therapist waits for the tissue to “melt.” The sensation is often a burning or stretching feeling that refers pain to distant areas along anatomical lines.
For instance, a patient with plantar fasciitis may have a root cause in the cervical fascia. Rubbing the foot provides temporary relief, but releasing the fascial tension in the neck alters the structural integrity of the entire system.
Clinical Logic: When to Use Which Therapy
At RSM, we rely on causal logic to select the right tool. We prioritize myofascial treatments when the tissue feels leathery or when postural deviations are fixed. If a client has scar tissue or chronic restrictions that do not respond to movement, we must address the container (fascia) before the contents (muscle).
Conversely, we prioritize deep tissue massage when the pain is localized to the muscle belly, such as DOMS after exercise, or when the tissue feels boggy and swollen. Here, the goal is circulation and parasympathetic down-regulation.
Anatomical Cascades and Causal Chains
To illustrate, consider the Levator Scapulae. It attaches to the upper cervical spine and the scapula. When a patient presents with a stiff neck, a standard approach targets the neck muscles. However, if the scapula is depressed due to a tight Pectoralis Minor, the Levator Scapulae is mechanically lengthened and under constant tension.
Massaging a “locked long” muscle aggravates it. The effective treatment is to apply myofascial expansion to the Pectoralis Minor. Releasing the anterior fascia allows the scapula to return to neutral, creating slack in the neck muscles. This causal chain connecting anatomy, biomechanics, and pain is the foundation of our curriculum.
Optimizing Movement and Structural Integrity
Ultimately, the choice between deep tissue work and myofascial release depends on the resistance of the tissue. Students often ask how much pressure typically is required. In massage therapy, pressure overcomes muscle tone. In myofascial release, pressure engages the barrier and waits.
Hironori Ikeda founded RSM to move beyond rote memorization. We teach that pain is a liar; the site of symptoms is rarely the source of the problem. Traditional massage chases symptoms, while structural integration corrects the cause.
Whether the goal is elite sports performance or general wellness, the therapist must decide: Are we flushing the engine, or are we repairing the chassis? By respecting the distinct physiology of the body, we strip away the restrictions that bind the human frame. This dual approach ensures our graduates deliver lasting results, restoring not just relief, but the potential for fluid movement.
Mastering Effective Stretching Techniques in Massage
Beyond Passive Stretching in Massage
Many therapists believe that simply pulling a limb creates flexibility. However, without engagement, stretching often triggers a protective reflex in the muscle spindles. This reaction causes the muscles to contract rather than relax, often exacerbating pain instead of relieving it. In RSM's Massage Workshops in Thailand, I emphasize that massage is not just mechanical manipulation; it is a neurological dialogue.
To be effective, we must respect the nervous system. Stretching techniques applied clinically must target the Golgi Tendon Organs to lower resting tone. If a therapist ignores these mechanisms, they are merely tugging on resistant structures. Therefore, the goal of any stretch within therapy is to obtain neurological permission for the tissue to lengthen.
Myofascial Release and Fascial Stretch
Force transmission occurs through the fascial network, not just independent muscle pulleys. When fascia is densified, a standard static stretch compresses the joint rather than elongating the tissue. For example, if the lateral thigh fascia is adhered, stretching the quad simply jams the knee.
To correct this, we utilize myofascial release before elongation. This prepares the tissue by creating a shearing force that restores sliding surfaces. This concept of fascial stretch focuses on the interface between compartments. We also prioritize pliability stretching, ensuring the tissue is hydrated and compliant. A shorter, pliable muscle is infinitely more functional than a long, stiff one. Combining stretch massage strokes with elongation encourages this hydration, offering superior results to dry stretching.
Implementing Resistance Stretching and Techniques
One of the most potent tools for correcting dysfunction is resistance stretching. By engaging the muscle eccentrically while it lengthens, we reorganize collagen and break down scar tissue. This active approach generates heat and re-educates the nervous system more effectively than passive methods.
We often integrate PNF stretching (Proprioceptive Neuromuscular Facilitation) to utilize post-isometric relaxation. Contracting a tight muscle against resistance loads the tendon, triggering an inhibition reflex that allows for a deeper range of motion. For athletes, dynamic stretching is also employed to maintain temperature and stimulate mechanoreceptors.
When integrating these methods, we follow a specific protocol to ensure the client retains the benefits:
- Preparation: Use massage to warm the tissue.
- Action: Apply assisted stretching techniques or PNF.
- Re-education: Have the client perform active movement to “save” the new range.
Advanced Isolated Stretching
Precision differentiates a general rub from clinical therapy. Isolated stretching targets specific muscle bellies rather than general chains. For instance, stretching the Psoas requires locking the lumbar spine to prevent compensation. If we fail to isolate, the force dissipates into hypermobile joints, potentially causing injury.
Assisted stretching techniques allow the therapist to control these vectors precisely. By stabilizing the pelvis, we can address a specific muscle like the Quadratus Lumborum without compromising the spine. This level of detail defines the curriculum at RSM. We do not view stretch therapy as separate from soft tissue work. They are symbiotic.
By combining flexibility protocols with anatomical precision, we do more than provide temporary relief; we improve long-term mobility. Therapists who master these techniques can solve complex pain patterns that standard treatments miss. Whether utilizing stretching assisted by pressure or active resistance, the focus remains on functional restoration.
Shiatsu Massage for Lower Back Pain
The Physiological Impact of Shiatsu
At RSM, we approach bodywork through the lens of sports medicine. While traditional modalities often focus on relaxation, the clinical application taught in our Shiatsu Massage Course requires a deeper understanding of physiology. Treating lower back pain requires more than generic contact. It requires precise manipulation of the nervous system and fascial layers.
When we apply perpendicular compression, we are not simply mashing muscle tissue. We are engaging the mechanoreceptors within the fascia to downregulate muscle tonus. This stimulation shifts the client from a sympathetic “fight or flight” state into a restorative state. For a person suffering from acute lower back tightness, this neurological reset is the prerequisite for structural change. Without addressing this neurological component, any massage is simply fighting against a guarded nervous system.
We often observe that local ischemia, or lack of blood flow, is a primary driver of discomfort in the low back. Static muscle contraction compresses capillary beds and prevents the evacuation of metabolic waste. The vertical force applied during shiatsu massage creates a temporary ischemic compression. This is followed by a rush of fresh, oxygenated blood upon release. This “pump mechanism” restores cellular health and pliability to the paraspinal muscles.
Decoding the Mechanism of Pain
To effectively treat the lumbar spine, a practitioner must look beyond the site of discomfort. The lumbar vertebrae are effectively the victims of a war being fought between the thoracic spine and the pelvis. We teach students to identify the causal chain rather than chasing symptoms of back pain.
A common pattern involves the Quadratus Lumborum (QL). When the QL becomes hypertonic, it pulls the pelvis into an anterior tilt or hikes the hip. This asymmetry forces the lumbar facets to jam together. This creates sharp, localized pain. However, the chain often extends further down.
Tight hamstrings are another frequent culprit. When the hamstring group is shortened, it pulls the ischial tuberosity downward. This creates a posterior pelvic tilt and flattens the natural lordotic curve of the lower back. A flat back loses its shock-absorbing capacity. This leads to bulging discs and nerve root compression. Therefore, massage therapy targeting the hamstrings is often more critical than rubbing the back itself. The lower back pain is merely the symptom of these biomechanical imbalances.
Precision Massage Protocols for the Back
In our courses, we emphasize that techniques must follow anatomy. The application of manual force aligns with specific anatomical landmarks. The Bladder Meridian, for instance, runs parallel to the spine and overlaps the Erector Spinae muscle group.
When treating the Erector Spinae, the therapist must locate the groove between the spinous processes and the muscle belly. Applying thumb compression here addresses the multifidus muscles. If these deep stabilizers are atrophied, the larger global movers overwork to compensate. This leads to fatigue and strain.
We utilize a specific sequence to address these layers. We begin at the sacrum to release the fascia, providing immediate slack to the spinal column. We then address the Ilio-Lumbar Ligament, a frequent site of chronic lower back inflammation. Finally, we target the Gluteus Medius and Minimus. Trigger points in these muscles refer sensations directly into the lumbar region. This methodical approach distinguishes professional shiatsu therapy from casual bodywork.
Evidence Supporting Massage Therapy
The medical community increasingly recognizes the value of manual manipulation. A study often validates what manual therapists have observed for centuries. Touch modulates pain perception via the Gate Control Theory. The non-painful input of touch inhibits the transmission of pain signals to the brain.
Research frequently compares a shiatsu group receiving targeted therapy against a control group. Results often indicate that the massage group experiences reduced cortisol and increased serotonin. Breaking the cycle of chronic discomfort requires a dual approach. We need mechanical release of soft tissue and chemical regulation of the brain’s pain matrix. At RSM, we integrate these findings into our curriculum to ensure our graduates practice evidence-based care.
RSM’s Clinical Approach to Massage
The distinction between a relaxation session and a clinical massage lies in assessment. Before a student at RSM lays a hand on a client, they must perform a visual and palpable assessment. We observe the client’s gait, their standing posture, and the rotation of their hips.
Our curriculum relies on the “thumb compression” technique. It allows for a level of diagnostic sensitivity that tools cannot replicate. Through the thumb, a therapist can detect changes in tissue temperature and texture. This sensory feedback guides the massage therapy in real-time. This dialogue between the practitioner and the client’s body is the essence of effective therapy.
Integrating Therapy and Movement
Recovery is rarely achieved through passive treatment alone. Passive care must be bridged with active movement. We encourage clients to engage in corrective exercises that support the work done on the table. Without neuromuscular re-education, muscles will often tighten again to provide artificial stability.
We also educate on the importance of “energy” efficiency in movement. A body that moves with aligned joints uses less metabolic energy and places less strain on ligaments. We may also suggest hand self-shiatsu for home care. Approaching pain massage as a partnership yields the best results.
For those interested in the professional application of these methods, the path requires dedication. A certification from RSM signifies that a therapist understands the intricate connections between the foot, the hip, and the spine. By addressing the root causes, we facilitate the body’s natural recovery process.
Mastering Assessment Protocols Used in Orthopedic Massage
Why Clinical Analysis Matters
In the field of sports medicine and remedial therapy, precision dictates success. Many therapists approach a client’s pain with a general routine, simply rubbing where it hurts. However, pain is often misleading. The site of the symptom rarely matches the source of the dysfunction. At RSM, we operate differently.
I teach students in our Orthopedic Massage Course that effective massage treatment relies entirely on accurate evaluation. If a therapist skips the investigation phase, the resulting therapy is merely a shot in the dark. It might provide temporary relaxation, but it will not resolve the biomechanical root cause. To elevate massage from simple relaxation to clinical rehabilitation, we must use structured protocols that guide our hands.
The Foundation: Subjective Patient History
The investigation begins with the history. The subjective interview acts as the first filter for our clinical reasoning. A client might report shoulder pain. A novice hears “shoulder” and thinks of the rotator cuff. I listen for the timeline. If the client mentions a severe ankle injury three years ago, my attention shifts to the lower limb.
That previous injury likely caused a gait alteration. The altered gait reduced gluteal activation, forcing the latissimus dorsi to compensate for pelvic stability. Since the lats insert into the humerus, the shoulder pain is actually a result of lower-limb instability. Without this assessment information, we treat the victim, not the criminal.
Visualizing Posture and Muscle Imbalance
Once we understand the narrative, we observe the structure. Static posture analysis provides visual cues about long-term imbalances. Muscles reshape the skeleton over time. If a muscle remains hypertonic, it shortens and pulls attachment points closer together.
Consider a high right iliac crest. The lumbar spine side-bends to the right to compensate. This compresses the facet joints on one side while placing the opposing muscles under eccentric strain. The client feels pain on the strained side, but the true pathology is the pelvic obliquity. If we simply apply deep massage to the painful side without addressing the pelvic tilt, we risk destabilizing the spine further.
Active and Passive Mobility Evaluation
Visual inspection gives us a map; testing tests the terrain. We must differentiate between inert tissues (capsules, ligaments) and contractile tissues (muscles). To do this, we utilize specific tests.
We begin with Active Range of Motion (AROM). If pain occurs, it is non-specific. Therefore, we move to Passive Range of Motion (PROM), where I move the joint while the client relaxes. If pain disappears during passive movement, the issue is likely a muscle or tendon, as the contractile unit is at rest. This is a green light for soft tissue therapy. However, if the pain persists or we hit a hard mechanical block, we suspect a joint capsule issue, requiring mobilization rather than standard massage.
Performing Orthopaedic Tests and Functional Movement
Beyond range of motion, we utilize orthopaedic tests to stress specific structures. A McMurray’s test checks for meniscus tears; a Straight Leg Raise tests for neural tension. These allow us to rule out conditions requiring medical referral.
We also analyze movement under load. During an overhead squat, if the knees collapse inward (valgus), it indicates weak gluteus medius muscles. This dynamic analysis reveals the “why” behind the pain, guiding our remedial planning.
The Art of Palpation
We confirm our logic with palpation assessment. This is where the hands become diagnostic tools. We look for T.A.R.T.: Tenderness, Asymmetry, Restriction, and Texture.
When I palpate, I evaluate resting tone. Is the tissue hypertonic (tight) or hypotonic (weak)? Many massage therapists mistake eccentric loading for tightness. In Upper Cross Syndrome, the rhomboids feel taut because they are “locked long” by tight pectorals. Digging into them only weakens the back further. My palpation confirms the tension, but biomechanics directs the treatment to the chest.
Designing the Orthopedic Massage Protocol
The orthopedic assessment dictates the plan. At RSM, we do not use routine sequences. If we find a capsular restriction, we use joint mobilization. If we find fascial adhesion, we use myofascial release.
We differentiate based on the recovery stage. In the acute phase, we use lymphatic drainage to reduce inflammation. In the chronic phase, we use friction techniques to break down scar tissue. The goal is not just relief, but the restoration of proper joint movement.
The Cycle of Re-Evaluation
Clinical therapy is a continuous loop. We assess, we treat, and we re-evaluate. If I apply a massage technique to the psoas, I immediately re-test hip extension. If the range improves, the hypothesis was correct.
This validation process separates a technician from a specialist. At RSM International Academy, we believe that the quality of the therapy is defined by the quality of the assessment. Without a map, you are lost. With a proper assessment, you have a direct path to recovery.
Understanding the Functional Differences Between Massage Modalities
Defining the Scope of Modern Massage Therapy
At RSM International Academy, we view the body as a biological machine. When students in our Deep Tissue Massage Course ask about the differences between massage modalities, they often expect a comparison of relaxation versus intensity. However, the distinction is mechanical. To be an elite therapist, you must understand the physiological chain of events your hands initiate.
When a client experiences chronic pain, the issue is rarely isolated. A biomechanical dysfunction triggers a protective spasm. This spasm reduces blood flow, causing hypoxia. Hypoxia creates acidity, which stimulates pain receptors. To treat this, we cannot simply rub the skin. We must intervene at the correct link in this chain.
Different massage styles intervene at different points. Some target the nervous system; others target fascial layers. Consequently, the massage therapy you choose determines the biological outcome. Knowing why you are touching a structure is more important than knowing how to touch it.
The Science Behind Various Massage Styles
To categorize massage, we look at the intent of the treatment. We generally divide bodywork into circulatory, structural, and neuromuscular categories.
Circulatory approaches, specifically Swedish massage, rely on venous return. Centripetal strokes push blood toward the heart. This increases cardiac preload, improving systemic circulation. Better circulation flushes metabolic waste, leading to reduced muscle tension.
In contrast, structural approaches focus on architecture. Deep tissue massage and myofascial release fall here. The goal is tissue elongation. Under sustained pressure, fascia changes from a gel to a fluid state. This restores the range of motion.
Neuromuscular approaches target the nerve-muscle connection. Techniques like trigger point therapy interrupt the pain-spasm cycle. We apply ischemic compression to cut off blood supply to a contracted sarcomere. Releasing the pressure floods the area with fresh blood, resetting the neuromuscular junction.
The type of massage dictates the mechanism. A skilled massage therapist switches tools instantly to suit the health needs of the client.
Swedish Massage vs. Structural Approaches
Swedish massage is the foundation of relaxation, but its effects are clinical. The technique stimulates skin mechanoreceptors, signaling the brain to downregulate the sympathetic nervous system (fight or flight). This lowers cortisol and systemic inflammation.
However, Swedish massage glides over fascia rather than engaging it. Structural styles differ. In structural work, we hook onto the tissue barrier. This engages the piezoelectric effect, generating a charge that signals fibroblasts to reorganize collagen. Over a session, this can reshape posture. Swedish massage relaxes muscles, but structural work realigns them.
Deep Tissue Massage and Neuromuscular Mechanisms
A pervasive myth suggests deep tissue massage is just Swedish massage with more force. Anatomically, this is incorrect. Deep tissue refers to the layer we target, not just the force we apply.
To access deep musculature like the quadratus lumborum, we must first relax superficial layers. If we apply heavy force immediately, the superficial muscles guard. Deep tissue massage requires a slow, sinking engagement to shear adhesions between muscle fibers. This restores the ability of muscle groups to slide past one another.
This leads to neuromuscular massage. While deep tissue focuses on layers, neuromuscular techniques focus on trigger points—hyper-irritable spots referring pain. We apply static pressure to create local ischemia. Upon release, a hyperemic response washes away pain-sensitizing chemicals. For therapists treating chronic pain, mastering this distinction is essential.
The Biomechanics of Thai Massage
Living in Chiang Mai, I respect Thai massage for its leverage systems. Unlike Western massage styles where the client is passive on a table, Thai massage uses yoga-like positioning on a mat.
The biomechanics are distinct. Passive stretching activates Golgi Tendon Organs (GTOs). GTOs detect tendon tension and inhibit muscle contraction to prevent tearing. By moving the client, the therapist utilizes these reflexes to gain range of motion.
Specific techniques utilize the practitioner’s body weight. Instead of using thumb muscles, I transfer force from my core. This results in deep, consistent pressure without practitioner fatigue.
Clinical Massage and Medical Applications
Clinical massage is a methodology, not just a technique. In a medical context, perhaps alongside a chiropractic doctor, our goal is functional improvement.
A session begins with assessment. We formulate a hypothesis—for example, tight hip flexors causing lumbar compression. The treatment focuses on lengthening specific muscles. We re-test immediately. If the range of motion improves, our hypothesis is confirmed.
This analytical approach differentiates a medical massage therapist from a spa practitioner. A chiropractic adjustment aligns bone, but if soft tissue remains tight, it pulls the bone back out of alignment. Soft tissue therapy is often the missing link.
Specialized Techniques: Lymphatic and Shiatsu
Lymphatic massage (or drainage massage) targets the lymphatic system, which relies on pressure changes to move fluid. Standard massage pressure collapses fragile lymphatic capillaries. Therefore, lymphatic massage uses extremely light traction to open capillaries and reduce edema.
Conversely, shiatsu massage applies rhythmic, static pressure to points corresponding to nerve bundles. This rocking motion stimulates the vestibular system, promoting deep relaxation distinct from deep tissue.
Integration and Training
The body adapts. If we use the same techniques, tissue builds tolerance. A therapist limited to one style cannot treat complex cases. A therapist only knowing deep tissue may injure a fibromyalgia patient.
At RSM, we emphasize that styles are tools. A session might start with Thai massage stretches, transition to deep tissue on the back, and end with lymphatic strokes. Integrating these differences between massage modalities leads to superior health outcomes.
Training determines your trajectory. You need training that explains the “why.” At RSM International Academy, we dissect these differences so graduates become engineers of the human body. Whether drawn to sports massage, the precision of Thai massage, or structural work, the foundation must be scientific.
By mastering the functional differences between massage modalities, you position yourself as a leader in wellness. The journey requires dedication, but the ability to resolve pain is the ultimate reward.
A Guide to Choosing the Right Massage Specialty
The Impact of Specialization
Generalist practitioners often struggle to build sustainable practices. There are many possible reasons. A therapist who attempts to master every modality rarely achieves the clinical depth required to solve complex musculoskeletal issues. Clients experiencing chronic pain do not seek a generalist, they seek an expert capable of identifying the root cause of their dysfunction.
As a specialized massage school in Thailand, RSM structures its curriculum around this reality. We observe that graduates who select a focused track early in their education achieve higher client retention rates. They understand anatomy not just as a diagram, but as a functional map of levers and pulleys. When a client presents with lower back pain, a generalist might simply rub the erector spinae. A specialist, specifically one trained in our sports medicine methodology, looks for the anterior pelvic tilt, tight hip flexors, and weak glutes that define lower-cross syndrome.
Selecting a massage specialty is not merely a preference. It is a strategic business decision that dictates the longevity and profitability of your career.
Massage Therapy vs Relaxation
Students must distinguish between recreational bodywork and clinical therapy. Relaxation massage has its place in stress reduction, but it rarely addresses the mechanical pathologies we see in a clinical setting. Students drawn to the therapeutic side of the industry often find pure relaxation work unfulfilling. They prefer the puzzle of pathology. They want to know why a muscle is hypertonic, not just how to soothe it.
Sports massage is the cornerstone of the RSM approach. This is not simply deep pressure applied to an athlete. It is a systematic manipulation of soft tissue to correct imbalances caused by repetitive motion. Consider the mechanics of a runner. They frequently suffer from lateral knee pain. A novice might label this as a local knee issue. A specialist understands the kinetic chain. The tension often originates in the Tensor Fasciae Latae (TFL), transmits through the iliotibial tract, and inserts at Gerdy’s tubercle. Treating the knee alone fails. Treating the TFL and correcting femoral mechanics succeeds.
Longevity and Biomechanics
Longevity in this field depends on biomechanics. Many therapists leave the profession within five years due to injury. They rely on thumb pressure and muscular effort rather than leverage and body weight. This is a failure of technique.
At RSM, Hironori Ikeda emphasizes a “therapist-first” approach to ergonomics. Deep work does not require self-sacrifice. When applying pressure to a dense structure like the gluteus medius, the therapist must stack their joints. They must generate force from their core and legs, not their wrists. A proper specialty education teaches you to use tools – elbows, knuckles, and forearms – to spare your thumbs.
The Science of Tissue and Assessment
To understand why specialization matters, one must understand the complexity of the soft tissue we treat. Muscles do not operate in isolation; they function in slings and chains. Effective therapy also respects the nervous system. “Deep” work that is too aggressive triggers a sympathetic response: fight or flight. The muscle tightens further to protect itself. We teach students to engage the parasympathetic system, using techniques that convince the nervous system to let go of the holding pattern.
You cannot treat what you cannot assess. Specialization requires mastery of orthopedic testing. Before a student touches a client at RSM, they perform a visual and functional assessment. We look for pelvic tilt, femoral rotation, and scapular position.
These observations dictate the treatment plan. If a client has an anterior pelvic tilt, we know the hip flexors are short and the hamstrings are long. We do not stretch the hamstrings, even if they feel tight. They are “locked long,” or eccentrically loaded. Stretching them further destabilizes the pelvis. Instead, we release the hip flexors to allow the pelvis to return to neutral. This logic is counter-intuitive to the untrained therapist, but second nature to the specialist.
The Financial Reality of Massage Therapy
Specialists command higher fees. The market recognizes skill. A therapist who can resolve a frozen shoulder or alleviate sciatica provides immense value. Clients are willing to pay a premium for results. In contrast, the general relaxation market competes on price. By choosing a niche in sports and rehabilitation, you remove yourself from the race to the bottom. You compete on quality and outcomes.
Choosing Massage Styles for a Career
The industry needs more thinkers. It needs more therapists who look at a swollen ankle and ask about hip stability. If you are content with a basic routine, a generalist path suffices. If you demand excellence from yourself and results for your clients, you must specialize.
At RSM International Academy, we provide the tools, the knowledge, and the mentorship.
Trigger Point Therapy for Athletes: A Sports Medicine Approach
Understanding the Science of Trigger Point Therapy
A common misconception is that muscle stiffness is always just “tightness.” In fact it is often a microscopic physiological error. Inside the muscle fiber, actin and myosin filaments lock together due to an excessive leak of acetylcholine. This sustained contraction compresses local capillaries, cutting off oxygen and trapping metabolic waste. The result is an acidic, ischemic environment that sensitizes pain receptors. We clinically define this hypersensitive nodule as a trigger point.
Trigger point therapy is not merely applying pressure; it is the reversal of this ischemia. By applying precise compression, as taught in our Trigger Point Therapy Course, we temporarily halt blood flow. Upon release, a hyperemic response floods the tissue with oxygenated blood, flushing out the acidic waste and allowing the sarcomere to unlock. This restores the muscle to its functional resting length.
How a Trigger Point Affects Biomechanics
A single nodule can destabilize an athlete’s entire kinetic chain. When a muscle harbors a trigger, it becomes functionally shorter and weaker. This forces surrounding structures to compensate, leading to injury far from the original site.
Consider a runner with a latent trigger in the soleus. This shortened calf muscle limits ankle dorsiflexion. To maintain forward momentum, the foot must pronate excessively, which forces internal tibial rotation and alters patellar tracking. As a result, athletes report lateral knee pain. A standard therapist might treat the knee, but at RSM, we treat the calf. The pain is the symptom; the restriction in the lower leg is the cause.
If we fail to map these referral patterns, treatment fails. An active trigger in the gluteus minimus often mimics sciatica, sending signals down the leg. By differentiating between nerve entrapment and a myofascial trigger, we ensure the body receives the correct intervention.
Differentiating Dry Needling from Manual Techniques
In modern sports medicine, techniques like dry needling have gained popularity. This involves inserting a monofilament needle into the taut band to elicit a spinal reflex that resets the muscle. While effective, invasive methods are not always the optimal starting point. Needling can cause significant post-treatment soreness, which may interfere with an athlete’s immediate schedule.
In contrast, manual trigger point massage offers diagnostic feedback that needles cannot. Through palpation, I assess tissue hydration, temperature, and fascial texture. While medical professionals may use point injections to numb the area, this masks the body’s feedback mechanisms. Manual therapy modulates the nervous system, reducing sympathetic tone and promoting the parasympathetic state required for deep recovery.
Integrating Trigger Point Massage into Training
Timing is critical. I teach my students that deep trigger point massage should never be performed immediately before a competition. Releasing a restriction drops muscle tone and alters proprioception. An athlete who feels “too loose” loses the elastic tension necessary for explosive performance.
Instead, we integrate this work during recovery phases. The goal is to maintain the ideal length-tension relationship in the muscles. A muscle at optimal resting length generates peak force; a shortened muscle creates less torque and fatigues rapidly. Therefore, pain relief is secondary to mechanical efficiency.
We also analyze sports specificity. Cyclists often develop shortened hip flexors, while pitchers overload the posterior shoulder. Recognizing these patterns allows us to treat trigger points proactively.
Common Athletic Trigger Sites:
- Upper Trapezius: Elevated by stress; refers pain to the head.
- Quadratus Lumborum: Strained by lifting; refers to the hip.
- Soleus: Shortened by running; refers to the heel.
Mastering Point Therapy for Long-Term Results
The difference between a silver and gold medal often lies in biomechanical efficiency. By understanding the physiology of myofascial trigger points, we move beyond treating symptoms and address the root of dysfunction. Whether using physical therapy modalities or manual compression, the objective remains the same: restore flow and function.
At RSM, we view the trigger as a map of the athlete’s history: their loads, compensations, and stress. Trigger Point therapy is the tool we use to read that map. When a therapist masters this logic, they stop just rubbing muscles and start optimizing the human machine for peak physical output.